TREATMENT
Overview
This topic covers management of arterial ulcers (AUs). For surgical management of arterial ulcers (AUs) with focus on surgical indications and selection criteria, see topic "Arterial ulcer - Surgical Treatment”. For an introduction and framework for assessment of arterial ulcers, including epidemiology, risk factors, etiology, pathophysiology, history, physical examination, diagnosis, differential diagnoses, documentation and ICD-10 coding, see topic "Arterial Ulcers - Introduction and Assessment". For clinical guidelines and quality measures, see topic "Arterial Ulcers - Overview". For a patient education handout, see topic "Patient Education - Arterial Ulcer"
Background
AUs are best managed by a multidisciplinary team as part of a comprehensive care plan.[5] In all practice settings, it is essential to ensure that the treatment plan and care provided adheres to the specific facility's policies, procedures, protocols, and formulary.
A customized treatment plan is created with the patient's input, based on a comprehensive assessment that:
- Identifies risk factors for development of AU and complications such as lower extremity amputation, delayed healing, and infections
- Differentiates from other types of lower extremity ulcers, which require different treatments
- Includes assessment by a vascular specialist who will:
-
- Assess the need for limb salvage or urgent drainage/debridement/amputation based on [1]:
- The patient’s perioperative risk and life expectancy,
- Limb severity staging, and
- Anatomical pattern of the disease
- Categorizes AUs using a lower extremity threatened limb classification staging system (e.g. The Society for Vascular Surgery Wound Ischemia and Foot Infection - WIfI classification system) that grades wound extent, degree of ischemia, and severity of infection to guide clinical management in all patients with suspected chronic limb-threatening ischemia (CLTI).
-
- Categorization helps determine the most adequate treatment plan. See ‘WIfI Classification System' in 'Algorithm 1' in topic "Arterial Ulcer - Introduction and Assessment" or in topic "Diabetic Foot Ulcers - Classification Systems"
- Determines ulcer prognosis or "healability", that is, the potential of the ulcer to heal.[6][7] Brief definitions are provided below. For details, see section 'Ulcer healability' in "Arterial Ulcers- Introduction and Assessment":
-
- Healable wound: the underlying cause of the ulcer can be conservatively or surgically corrected, blood supply is enough to heal the wound or can be restored, existing co-factors, conditions or medications that could delay healing can be optimized or ideally corrected.
- Maintenance wound: the wound may be healable, but the cause cannot be corrected due to patient’s unwillingness to adhere to treatment or a lack of required system resources.
- Non-healable wound: the patient is severely ill (e.g. major organ failure), has a high surgical risk, or the AU is caused by inadequate blood supply that is not bypassable or dilatable, or the risk-benefit ratio for the probability of revascularization success is unfavorable, or unclear.
See section ‘Indication’ in topic “Arterial Ulcer - Surgical Treament”.
- Determines if the patient needs to be admitted to the hospital or can be treated in an outpatient setting.
An adequate treatment plan for AUs aims to [6]:
- Treat the cause and other factors impeding healing
- Assess patient's and caregiver's concerns
- Provide effective local wound care
Patients with healable AUs should undergo either prompt revascularization or a 4-week trial of conservative treatment followed by revascularization, depending on the WIfI classification. [1] See Algorithm for Management of Arterial Ulcers (Algorithm 1) and section 'Management of arterial ulcers by healability and limb severity' below.
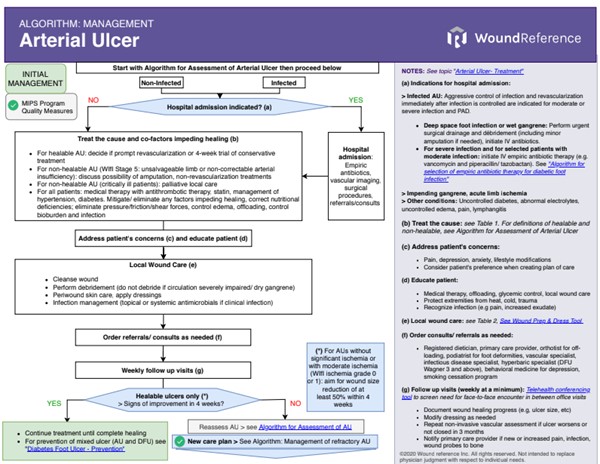
Algorithm 1. Algorithm for Management of Arterial Ulcers (click link to enlarge)
Treatment Goals
Treatment goals are determined in conjunction with the patient and caregivers and are guided by healability and patient concerns. For best results, patient-driven goals should be developed based on SMART (Specific, Measurable, Attainable, Relevant, Timely) principles.[8]
Patients with AU and deep space foot infection or wet gangrene
- For all patients with AU and deep space foot infection or wet gangrene, the initial treatment goal is infection control.
-
- Refer to a vascular specialist or surgeon with experience in CLTI for urgent surgical drainage and debridement (include minor amputation if needed).[1]
-
- Repeat limb staging (e.g. with WIfi) after surgical drainage, débridement, minor amputations, and before the next major treatment decision.[1]
Healable AUs
- For healable AUs, treatment goals include ischemic and ulcer pain relief, wound healing, preservation of a functional limb, prevention of recurrence, and reduction of cardiovascular morbidity and mortality through aggressive risk factor modification and medical management. [1][2]
-
- In patients with healable AUs, restoration of blood flow by revascularization combined with medical therapy, edema control, offloading and local wound care are the interventions that will most likely lead to healing.[1][2]
- Risk factor modification includes management of modifiable risk factors such as hyperlipidemia, hypertension, diabetes, smoking, and sedentary lifestyle.[1][2]
- For patients who have undergone successful revascularization, goals include wound closure (e.g. within 3 months following revascularization), monitoring of potential re-stenosis by vascular specialist, prevention of wound infection, trauma and pressure injury.[8]
Non-healable or maintenance AUs
- For non-healable or maintenance AUs, palliative wound care goals include prevention of ulcer progression and complications, pain relief, bioburden control. Patient's concerns and comfort should be prioritized when creating a treatment/care plan.
-
- For patients with non-healable AUs (i.e. with limited life expectancy, poor functional status, or an unsalvageable limb after shared decision-making), palliation or primary amputation may be offered.[1]
Management of arterial ulcers by healability and limb severity
Patients with healable AUs should undergo prompt revascularization or a 4-week trial of conservative treatment potentially followed by revascularization, depending on the WIfI classification.[1] See WIfI classification in 'Algorithm 1'.
- Vascular specialists’ decision on whether to offer revascularization is based on patient factors (i.e., perioperative risk and life expectancy) and limb condition (i.e., limb severity and anatomy).[1]
-
- The higher the degree of ischemia and severity of limb threat, the higher the likelihood that a patient with a healable AU will benefit from revascularization.
- Figure 1 illustrates the estimated benefit from revascularization for each WIfI stage. Table 1 depicts management of AUs by healability and limb severity. In summary:
-
- For healable AUs without significant ischemia (WIfI stage 1 with WIfI ischemia grade 0) or with moderate ischemia and intermediate limb risk (WIfI Stage 2 or 3 with WIfI ischemia grade 1), clinicians might opt for a 4-week trial of conservative treatment.
- All healable AUs undergoing conservative treatment should be reassessed for signs of improvement after 4 weeks of appropriate interventions (i.e. infection control, wound care, and offloading).
- For patients with mild-to-moderate ischemia and tissue loss, a conservative approach has been shown to achieve complete wound healing in 76.8% of limbs in 4.4 ± 4.1 months; and limb salvage at long-term follow-up of 89.3%, with limited need for deferred revascularization (14%).[9][10][11]
- If the ulcer does not decrease in size by 50% in 4 weeks despite appropriate interventions, clinical guidelines suggest revascularization for the following cases [1]:
- AUs with moderate ischemia (WIfI ischemia grade 1) and intermediate limb threat (WIfI stages 2 and 3)
- AUs without significant ischemia (WIfI ischemia grade 0), but with an isolated region of poor perfusion in conjunction with major tissue loss (eg, WIfI wound grade 2 or 3)
- For all other patients with no significant ischemia (WIfI ischemia grade 0) revascularization is not recommended
- For patients with more severe ischemia and/or tissue loss and/or infection, prompt revascularization should be considered. Care coordination between wound care and vascular specialists is essential in caring for patients and their ulcers before and after surgical interventions.
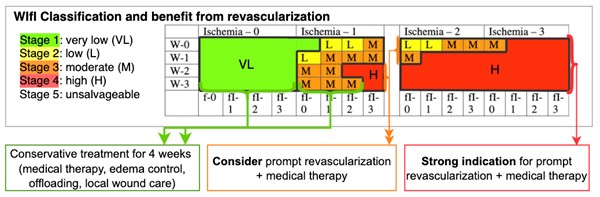
Fig. 1. Interventions and estimated benefit from revascularization for each WIfI stage
Table 1. Management of AUs by healability and limb severity
|
Infected AU
|
|
Infected AU
|
Treat the cause
Higher risk of amputation, especially if neuroischemic ulcer. Evaluate need for hospital admission:
- If infection is severe (systemic signs of infection, deep space foot infection, wet gangrene - i.e. WiFI Foot Infection 3), patient should be treated as a medical emergency with immediate drainage, debridement, culture, systemic antibiotics and consideration for revascularization.[1][5][12]
-
- Collect wound culture and initiate empiric antibiotic treatment (e.g. vancomycin and piperacillin/ tazobactan). Adjust antibiotics based on culture results. See 'Algorithm 1' in topic "Diabetic Foot Ulcer Associated with Infection - Management"
- For patients with hemodynamic instability, immediate amputation may be the only option.[13]
- If infection is non-limb-threatening, blood supply to the foot should be optimized before surgical debridement to ensure that potentially viable tissue is not unnecessarily removed.[13]
-
- Collect wound culture and initiate empiric antibiotic treatment, adjust antibiotics based on results and signs of improvement
- If AU does not respond with interventions to treat infection (e.g. antibiotics, abscess drainage) or if there is deterioration, revascularization should be strongly considered
|
Local wound care
- Antimicrobial dressings
- If infection is severe: surgical referral needed for consideration of surgical debridement
- If infection is non-life threatening: optimize blood supply prior to surgical debridement. Careful removal of debris and non-viable tissue may be performed, if arterial perfusion to the AU is considered sufficient to promote wound healing with conservative treatment (e.g. ABI > 0.6 or TcPO2> 40mmHg)
|
Revascularization
See ‘Treat the Cause’ on the left.
|
|
Healable ulcer
|
|
Very low limb risk
(WIfI stage 1)
|
Treat the cause
- Management of underlying conditions
- For patients with CLTI: medical therapy and aggressive risk factor management (antithrombotic therapy, lipid lowering therapy, management of hypertension and diabetes, tobacco cessation)
- Nutrition optimization
- Foot, callus and nail care
- Edema control
- Offloading
- Infection and bioburden control
|
Local wound care
- For healable AUs: cleansing, conservative debridement, infection and bioburden control, periwound care, moisture balance
|
Revascularization
- For AUs without significant ischemia (WIfI ischemia grade 0), but with an isolated region of poor perfusion in conjunction with major tissue loss (eg, WIfI wound grade 2 or 3), consider revascularization if the wound progresses or fails to reduce in size by at least 50% within 4 weeks despite appropriate care
- For all other patients with no significant ischemia (WIfI ischemia grade 0) do not perform revascularization
- 2CFor AUs with moderate ischemia (e.g, WIfI ischemia grade 1) consider revascularization if the wound progresses or fails to reduce in size by > 50% within 4 weeks despite appropriate care. (Grade 2C)
|
|
Intermediate limb risk
(WIfI stage 2, WIfI stage 3)
|
Treat the cause
- Management of underlying conditions
- For patients with CLTI: medical therapy and aggressive risk factor management: antithrombotic therapy, lipid lowering therapy, management of hypertension and diabetes, tobacco cessation
- Nutrition optimization
- Foot, callus and nail care
- Edema control
- Offloading
- Infection and bioburden control
|
Local wound care
- If arterial perfusion to the AU is considered sufficient to promote wound healing with conservative treatment (e.g. ABI > 0.6 or TcPO2> 40mmHg): conduct cleansing, conservative debridement, infection/bioburden control, periwound care, moisture balance
- If insufficient blood flow to heal (e.g., limb pending revascularization):
-
- Do not use moisture-retentive and occlusive dressings (e.g. hydrogel, hydrocolloid)
- Use non-adherent dressings, foam dressings
|
Revascularization - 2CFor AUs with moderate ischemia (e.g, WIfI ischemia grade 1) consider revascularization if the wound progresses or fails to reduce in size by > 50% within 4 weeks despite appropriate care. (Grade 2C)
- 2CFor AUs with significant ischemia (e.g., WIfI ischemia grades 2 and 3), consider prompt revascularization (Grade 2C)
|
|
Advanced limb-threatening conditions
(WIfI stage 4)
|
Treat the cause
- Management of underlying conditions
- For patients with CLTI: medical therapy and aggressive risk factor management
- Nutrition optimization
- Pain management
- Foot, callus and nail care
- Edema control
- Offloading
- Infection and bioburden control
|
Local wound care
- Avoid moist wound healing
- Keep clean and dry
- Apply povidone-iodine daily
|
Revascularization
- 2CFor AUs with moderate ischemia (e.g., ischemia grade 1), prompt revascularization is suggested (Grade 2C)
- 1CFor AUs with significant perfusion deficits (e.g. ischemia grades 2 and 3), prompt revascularization is strongly recommended (Grade 1C)
|
|
Non-healable or maintenance ulcers
|
|
Any WIfI stage
|
Treat the cause
- Management of underlying conditions
- For patients with CLTI: medical therapy and aggressive risk factor management
- Nutrition optimization
- Pain management
- Foot, callus and nail care
- Edema control
- Offloading
- Infection and bioburden control
|
Local wound care
- Keep AU dry
- Do not debride
- Apply povidone-iodine daily
|
Revascularization
Palliation rarely includes revascularization, except in special cases such as [1]:
- To improve the likelihood of a successful amputation at the most distal possible level
- To relieve intractable pain
|
Treat the cause and co-factors impeding healing
As mentioned, for patients with healable AUs due to CLTI, revascularization in combination with medical therapy, risk factor management, edema control, offloading, infection control, and local wound care are the interventions that will most likely lead to healing.[1][2]. Those interventions are detailed below. For revascularization techniques, see topic “Arterial ulcer - Surgical Treatment”
Medical therapy
CLTI is an end-stage manifestation of systemic atherosclerosis. Best medical therapy and aggressive risk factor modification will not only salvage a functional limb, but also reduce cardiovascular morbidity and mortality. Risk factors such as age and sex cannot be modified, but others can, including hyperlipidemia, hypertension, diabetes, smoking and sedentarly lifestyle.[1]
Antithrombotic therapy
- 1AFor all patients with AUs due to CLTI, clinical guidelines recommend administration of an antiplatelet agent to reduce the risk of major adverse cardiovascular events. (Grade 1A) [1]
- 2BConsider 75 mg of clopidogrel per day as the single antiplatelet agent of choice in patients with CLTI (Grade 2B).[1][5]
-
- Rationale: A meta-analysis that reviewed the use of aspirin, ticagrelor, ticlopidine, cilostazol, picotamide, vorapaxar, and clopidogrel as single antiplatelet therapy or dual antiplatelet therapy (DAPT) in patients with PAD found that clopidogrel monotherapy resulted in the best overall safety and efficacy.[14][15][1]
Lipid lowering therapy
- 1AFor all patients with AU due to CLTI, clinical guidelines recommend use of moderate- or high-intensity statin therapy to reduce all-cause and cardiovascular mortality (Grade 1A) [1][16]
-
- Rationale: High-intensity/ maximally tolerated statin dosing is recommended. Guidelines recommend low density lipoprotein (LDL-C) target of < 1.8 mmol/L (< 70 mg/dL) and reduction by at least 50% of baseline. Both rosuvastatin (20-40 mg) and atorvastatin (40-80 mg) have been shown to be effective in reducing all-cause and cardiovascular mortality [17]. In addition, if LDL-C levels remain >70 mg/dL (1.8 mmol/L), ezetimibe (a cholesterol absorption inhibitor) may be added.[1][16] If high intensity statin therapy (with or without ezetimibe) is tolerated, target levels < 1.4 mmol/L (55 mg/dL) are recommended.[5]
Management of hypertension
- 1BFor all patients with AU due to CLTI, clinical guidelines recommend controlling hypertension to target levels of < 140 mm Hg systolic and < 90 mmHg diastolic to reduce major adverse cardiovascular events (Grade 1B).[1][5][16]
-
- Rationale: Typical drugs include diuretics, angiotensin-converting enzyme inhibitors (ACEIs), angiotensin II receptor blockers (ARBs), and calcium channel blockers. As long as successful in lowering blood pressure to target, these drugs seem to reduce cardiovascular events to a similar extent. [18]
Management of diabetes
For all patients with AU with type 2 diabetes mellitus, glycemic control is essential to reduce cardiovascular risk and the extent of vascular disease. [1][16]
- 1BFor patients with healable AUs and type 2 diabetes mellitus, we recommend intensive glucose control (HbA1c, 6%-7.5%) over less intensive glycemic control to reduce risk of lower extremity amputation, if this can be achieved without significant hypoglycemia (Grade 1B).[19]
-
- Rationale: There is moderate certainty evidence that compared with conventional glucose control, intensive glucose control is significantly more effective in decreasing risk of amputation in patients with DFU (evidence level B). [1][20]
- For patients with non-healable AU and type 2 diabetes mellitus, clinical guidelines suggest less stringent goals (eg, hemoglobin A1c level < 8%).[1][5][19][20]
- 1AFor all patients with AU and type 2 diabetes mellitus, clinical guidelines recommend use of metformin as the primary hypoglycemic agent (Grade 1A).[1][21]
-
- Rationale: When additional therapy is needed, any other class of oral hypoglycemic agent, including sulfonylurea, thiazolidinedione, dipeptidyl peptidase 4 inhibitor, oraglucosidase, can be added with equal effectiveness.[21]
Lifestyle modifications
- 1ATobacco: For all patients with AU who smoke or use tobacco products, clinical guidelines recommend offering smoking cessation interventions (pharmacotherapy, counseling, or behavior modification therapy) to reduce major adverse cardiovascular events (Grade 1A).
-
- Rationale: Even smokers who smoke 1 cigarette per day have a significantly increased rate of disease progression and major cardiovascular events when compared to non-smokers.[22]
- Pharmacotherapy for smoking cessation: Evidence supports use of nicotine replacement therapies (gum, patch, spray, lozenge, and inhaler), selected antidepressant therapies (e.g., bupropion), and nicotinic receptor agonist therapy (varenicline), which have been shown to result in better smoking cessation rates than placebo.[23]
- Diet: For all patients with AU, clinicians might opt for encouraging patients to adopt a low-fat or Mediterranean diet to reduce atherosclerosis and major cardiovascular adverse effects.[1][21]
-
- Rationale: There is compelling evidence that diet affects the progression of atherosclerosis. Diets with low intake of saturated fats, and higher intake of monounsaturated fats, omega-3 fatty acids and other natural plant sterols and stanols are associated with a reduction in plaque burden and major cardiovascular adverse effects.[1][21]
- Exercise: For all patients with AU who have undergone revascularization and are cleared for full-weight bearing, walking-based exercise program is suggested.[1][21]
Foot, callus and nail care
Self-care routine should include:
- Daily foot and shoe inspection,
- Daily foot washing (with careful drying particularly between the toes),
- Avoidance of chemical agents or plasters to remove callus or corns,
- Use of emollients to lubricate dry skin
- Cutting toenails straight across
Edema control
- For patients with ulcers of mixed etiologies (venous and arterial), guidelines suggest use of modified or no compression therapy to support wound healing.[24]
-
- Rationale: Edema may interfere with blood perfusion, delaying the healing process. Compression therapy utilizing lower levels of compression helps minimize edema.
Prior to applying compression, objective evidence with non-invasive arterial tests (e.g. ABI, audible handheld doppler, etc) should be obtained that the arterial supply is sufficient and it is safe to apply compression. See topic “How to Select Adequate Compression Therapy Pressure Levels and Products”
- For patients with AU who have undergone surgical revascularization, clinicians might opt for mild compression to reduce postoperative edema and promote wound healing, if approved by the surgeon.[24][3]
-
- Rationale: After bypass surgery, postoperative edema is relatively common and compression therapy with graduated compression stockings (18-30 mm Hg) is often helpful.[24] Excessive compression should be avoided, and pain should be monitored.
Offloading
For all patients with AUs (especially those with associated peripheral neuropathy), a biomechanical assessment by a specialist (podiatrist, orthotist) is recommended in order to determine a proper offloading strategy and promote healing and prevent new ulcers. [8]
- Foot protection and pressure offloading is essential in preventing trauma, pressure ulcers/injuries, and ulceration.[3]
Several offloading devices exist, and a few options are listed below. For details, see topics “Diabetic Foot Ulcer - Treatment" and "How to Select Offloading Devices":
- For severely infected AUs: non-removable knee high devices (total contact case or irremovable cast walkers) are not recommended, as these impair frequent ulcer inspections.
- For AU patients with mild PAD or mild infection under control with antibiotics: non-removable knee-high devices may be an option. For other patients with infected or ischemic DFU, removable cast walkers may be used and are preferred over half shoes.
Infection control
Patients with infected AUs are at particularly high risk for major limb amputation, especially if the ulcer is neuroischemic (i.e. mixed neuropathic and ischemic diabetic foot ulcer). [5][12] Assessment of perfusion status and evaluation by a vascular specialist are recommended.
Interventions for infection control include systemic antibiotics, local wound care with antimicrobial dressings, debridement, surgical drainage, and revascularization.[24] For local wound care of infected AUs, see section ‘Local wound care - infection and bioburden control’ below.
- 1CFor patients with AUs and suspected limb infection, guidelines recommend immediate evaluation by vascular specialist, assessment of perfusion status and culture-guided antibiotic therapy (Grade 1C).[5][12][24]
-
- Rationale: Infection of ischemic ulcers is a primary risk factor for major amputation.[1][5][12]
- The need for hospital admission, intravenous systemic antibiotics and immediate surgical debridement/ drainage should be evaluated:
-
- If infection is severe (systemic signs of infection, deep space foot infection, wet gangrene - i.e. WiFI Foot Infection 3), patient should be treated as a medical emergency with immediate drainage, debridement, culture, systemic antibiotics and consideration for revascularization.[1][5][12]
-
- Prompt Initiation of empiric antibiotic treatment (e.g. vancomycin and piperacillin/ tazobactan) is recommended. See 'Algorithm 1' in topic "Diabetic Foot Ulcer Associated with Infection - Management"
- For patients with hemodynamic instability, immediate amputation may be the only option.[13]
- If the infection is non-limb-threatening, blood supply to the foot should be optimized before surgical debridement to ensure that potentially viable tissue is not unnecessarily removed.[13]
Systemic antibiotics
- 1CFor infected AUs, clinical guidelines recommend clinicians obtain culture and start empiric antibiotic regimen on the basis of the severity of the infection and the likely etiologic agents, and then implement definitive therapy based on the culture and sensitivity results, and the patient’s clinical response to the empiric regimen (Grade 1C) [24]
-
- Rationale: Infected AUs can turn into a limb and life-threatening condition, and must be treated promptly. For infected AUs, topical antimicrobials alone are not sufficient.[8] Clinical guidelines [24][25] recommend starting empiric antibiotic regimen after a specimen for culture is properly collected, and adjusting the regimen based on culture and sensitivity results and response to the initial course of antibiotics.
Of note, antibiotic therapy alone is insufficient, unless combined with standard care (e.g. medical therapy, local wound care, offloading, etc).
- For guidance on empiric antibiotic selection for infected AUs, see topic "Diabetic foot ulcer Associated with Infection - Management)
- Prior to initiating any antimicrobial therapy, clinicians should obtain wound culture. If there is suspicion for systemic infection, blood culture should be obtained.
-
- Guidelines suggest use of tissue biopsy, considered the gold standard, to confirm a diagnosis of infection. Alternatively, non-invasive quantitative swab cultures using the Levine technique may be used.[24] See section 'Diabetic Foot Infection' in topic "Diabetic Foot Ulcer - Introduction and Assessment".
- Of note, if resolution of infection is delayed despite systemic antibiotic therapy and adequate care, there might not be enough blood (and antibiotic) reaching the affected areas. Prolonged outpatient antibiotic therapy may decrease the chance of wound healing and limb salvage. In these cases, infection will be better managed in an environment with adequate blood supply, thus vascular evaluation for consideration of revascularization is recommended. [3]
Osteomyelitis management
- For osteomyelitis assessment, see section ‘Osteomyelitis’ in "Diabetic Foot Ulcer - Introduction and Assessment"
- For management, see topic "Diabetic Foot Ulcer Associated with Infection - Management"
Address Patient Concerns
Pain management
For all patients with AU, pain should be adequately managed to improve quality of life and functional capacity.
- Rationale: patients with AU experience significant levels of pain, which can lead to depression and decreased ability to carry out routine activities. A tiered approach to pain management is recommended by clinical guidelines. [1]
- Surgical revascularization is the most effective way to reduce ischemic pain, as it addresses the underlying cause of the pain.[3] Of note, patients may experience temporary reperfusion pain after revascularization.
- Analgesics: clinicians might opt to follow the World Health Organization (WHO) Pain Ladder for cancer patients, with modifications for wound care. Benefits and harms of each step should be considered. In summary [26] :
-
- Step 1: A non-opioid analgesic (e.g., NSAID) with or without an analgesic adjuvant. Adjuvants include tricyclic antidepressants, anticonvulsants, antihistamines, benzodiazepines, steroids, and phenothiazines.
- Step 2: If pain is not controlled: Continue the initial medication and add an opioid, such as codeine or tramadol, and an adjuvant
- Step 3: If pain is not controlled: discontinue second step medications and initiate a more potent oral narcotic
- Insulated offloading boot may be used to protect, offload, and insulate the extremity. Findings of a pilot study suggested that continued insulated offloading therapy increased local skin temperature and tissue perfusion via vasodilation, thereby reducing pain. [27]
Depression
For all patients with AU, we suggest referral to behavioral medicine for screening and management of depression.[28][29]
- Rationale: Depression is highly prevalent among patients with CLTI (~36%).[28] Depression symptoms seem to significantly improve immediately after limb revascularization. A decrease in depression symptoms compared to baseline has also been observed 6-12 months after major amputation, possibly due to the fact that patients experienced chronic ischemic limb pain before amputation.[28]
Local Wound Care
For all patients (healable, non-healable, maintenance), appropriate local wound care should be implemented to avoid infection and further injury.[3] Table 2 summarizes local wound care interventions for healable and non-healable/maintenance AU.[6][24][3][30] Evidence and recommendation for each intervention are listed after the table. For customized, wound-specific recommendations, use Wound Prep and Dress Tool.
Table 2. Local Wound Care for Arterial Ulcers
|
|
Healable
|
Non-healable/ maintenance
|
|
Cleansing
|
-
For AUs with sufficient blood perfusion to heal, gently cleanse with normal saline, sterile water or commercial wound cleanser. Irrigate wound with > 100 mL of room/body temperature solution at low pressure (4-15 psi)
- For AU with non-infected blisters, dry gangrene or eschar: keep dry until revascularization is successful
|
|
|
Debridement
|
- For foot infections involving wet gangrene, abscess, gas, or necrotizing fasciitis: urgent surgical debridement is recommended
- Dry gangrene or stable black eschar should not be debrided
- For other AUs, obtain objective evidence that AU is healable prior to debridement (e.g. ABI > 0.6 or TcPO2 > 40mmHg):
-
-
Debridement may be conservative sharp, mechanical, autolytic, enzymatic, or a combination of methods.
-
Do not use enzymatic or autolytic methods for infected AUs. For non-infected AUs, closely monitor AU if either method is employed
|
|
|
Infection and bioburden control
|
-
Use antimicrobial dressings only in cases of clinical infection or if no healing is seen despite appropriate care
-
Antimicrobial dressings (e.g. with cadexomer iodine, silver, etc):
-
-
For light exudate: non-adherent dressing
-
For moderate, heavy exudate: alginate, fiber gelling dressing (hydrofiber),specialty absorptive
-
If clinical infection, collect wound culture, initiate empiric antibiotic therapy and adjust based on culture results
-
Surgical referral needed for deep infection, abscess, compartment syndrome, wet gangrene (e.g. necrotizing fasciitis)
|
-
If minimal or light exudate, consider antiseptic solution (e.g. povidone iodine, chlorhexidine)
-
If moderate or heavy exudate, consider non-adherent antimicrobial dressings (with cadexomer iodine, silver, etc)
-
If signs of clinical infection, collect culture, prescribe empiric antibiotics, then adjust according to culture results
-
If life-threatening infection (e.g. gas gangrene or necrotizing fasciitis), the patient may need limb amputation.
|
|
Periwound skin care
|
-
Protect the periwound skin:
-
- Prepare the skin prior to dressing application with skin barrier wipes that form protective film layer
- Opt for adhesive tapes made of soft silicone when securing dressings
-
If dry skin, apply humectants and/or emollients for skin hydration. Do not apply those products on the wound
|
- Avoid all sources of moisture, such as foot soaks, creams and ointments, to reduce risk of infection
|
|
Moisture balance
|
Check AU arterial perfusion:
-
If perfusion status is unknown, follow the non-healable/maintenance program until arterial testing is performed
-
If arterial perfusion is considered sufficient to promote AU healing:
-
- If arterial perfusion is considered insufficient blood flow to heal (e.g., limb pending revascularization):
-
- Do not use moisture-retentive and occlusive dressings (e.g. hydrogel, hydrocolloid)
- Use non-adherent dressings, foam dressings
|
-
Apply appropriate non-adherent dressing OR
-
If minimal or light exudate: paint daily wound with antiseptics (e.g. povidone iodine)
-
If dry or wet gangrene: do not use moisture-retentive dressing, as it may cause limb threatening infection
-
Avoid conventional dressing products that require daily dressing changes
|
Cleansing
-
2CFor healable, non-infected AU with enough blood perfusion to heal, we suggest cleansing with a neutral, non-irritating, non-toxic, non-antimicrobial solution such as sterile saline or water initially and at each dressing change, and that routine wound cleansing be accomplished with a minimum of chemical and/or mechanical trauma (4-15 psi of pressure) (Grade 2C).[24][30]
- Rationale: Although there is minimal evidence that routine cleansers can result in improvement of AUs, and Medicare part B does not cover wound cleansers, AUs frequently have biofilm and debris in and around the wound area, which must be cleansed before debridement or dressing application.
-
- For AU with non-infected blisters, dry gangrene or eschar, cleansing is not recommended.[24][3][30]
-
- Rationale: Irreversible tissue loss such as dry gangrene or eschar should be left dry. The addition of moisture to necrotic tissue may create an environment that facilitates bacterial growth and infection. [3]
Debridement
- For AUs with wet gangrene, abscess, gas, or necrotizing fasciitis, surgical debridement prior to revascularization is indicated in order to control infection. [24][3]
- For AUs with dry gangrene or black stable eschar, debridement is not recommended.[24][3]
-
- Rationale: Irreversible tissue loss such as dry gangrene or eschar indicates poor tissue oxygenation. Removal of dry gangrene or eschar can result in further necrosis and infection. If the patient is a candidate for revascularization, debridement should not be performed until after arterial inflow has been reestablished and patient is under appropriate antibiotic coverage. [3]
-
For healable AUs without dry/wet gangrene or eschar, careful debridement of non-viable tissue may be performed, however clinicians should obtain objective evidence that the AU is healable before debriding the ulcer.[24][3] See section 'Noninvasive arterial tests' in topic "AU Intro and assessment"
-
- Rationale: Debridement of an AU with insufficient blood perfusion to promote healing can lead to enlargement of the wound and spread of infection.[3]
- Debridement methods for healable AUs include surgical, conservative sharp, mechanical, enzymatic, or autolytic methods. If autolytic or enzymatic debridement methods are used, carefully monitor wound for signs of infection.[24]
-
- When choosing debridement methods, it is important that clinicians take into account relative contraindications such as severe ischemia, clinical context, availability of expertise and supplies, patient tolerance and preference, cost-effectiveness, professional licensing restrictions and insurance coverage. See topic “Debridement”
- Debridement methods include:
-
- Surgical debridement: may be performed after arterial inflow is reestablished.
- Conservative sharp debridement with curette, scissors, scalpel, and forceps. See topic “How to Perform Conservative Sharp Wound Debridement”
- Enzymatic debridement: for patients who cannot tolerate sharp debridement or if resources are not available. If used on AU, carefully monitor wound for signs of infection.[24] See topic "Products that inhibit collagenase enzymatic activity".
- Autolytic debridement (e.g.,hydrogels, hydrocolloid): moisture-retentive dressings are not recommended for patients with ischemia and/or dry gangrene.[32] If used on AUs, wound should be closely monitored for signs of infection. [24]
- For non-healable AUs, debridement is contraindicated. [24]
-
- Removal of necrotic tissue can result in further necrosis, ulcer enlargement and infection.[24]
Infection and bioburden control
Infection in AUs can be challenging to identify, as signs and symptoms are often muted due to decreased perfusion. The need for hospital admission, systemic antibiotics and immediate surgical debridement/ drainage should be evaluated promptly. See sections ‘Ulcer Complications' in topic "Arterial Ulcer - Introduction and Assessment", and section ‘Treat the cause - Infection Control’ above.
- For healable AUs, interventions to manage infection include topical antimicrobial dressings, systemic antibiotics and debridement:
-
- For superficial infections, topical antimicrobial dressings are indicated to decrease bacterial load and aid wound healing.[3] However, topical antimicrobials alone are not sufficient to treat an infected AU.[8] Clinical guidelines recommend that patients with AUs be promptly treated with systemic antibiotics in addition to topical antimicrobials.[8][24][33]
-
- Superficial infections can be recalled by the NERDS mnemonic: Non Healing, Exudate, Red-friable tissue, Debris, Smell. If 3 or more are identified, topical antimicrobial dressings are indicated.
- Among topical antimicrobial dressings, clinicians might opt for dressings with ionized silver dressings, polyhexamethylene biguanidine, honey products, cadexomer iodine, or methylene blue/gentian violet
- Use of antimicrobial dressings should be assessed weekly and discontinued once signs of infection have improved or after 4 weeks in the absence of signs of improvement.[3]
- Topical antibiotics should be avoided in order to prevent bacterial resistance and patient sensitization.[3]
- For deep, spreading and/or systemic infections, systemic antibiotics are recommended, in addition to topical antimicrobial dressings.[3]
-
- Deep and surrounding infection: The STONEES mnemonic (Size, Temperature, Os, New breakdown, Exudate, Erythema + edema (cellulitis), Smell) can help identify deep and surrounding infection. Systemic antibiotics and topical antimicrobial treatment are justified if 3 or more of the STONEES signs are present.
- For non-healable/maintenance AUs that are infected, keeping the ulcer dry, topical antiseptic agents (e.g., povidone iodine or chlorhexidine), and systemic antibiotics are usually appropriate.[3] A nonviable limb with a potentially life-threatening infection (e.g. gas gangrene or necrotizing fasciitis) may need amputation. [3]
Peri-wound Care
- For all patients with AU, care must be taken to avoid skin injuries due to tape and adhesive products, as skin is often fragile.
-
- Adhesive products made of soft silicone are preferred as they are less likely to cause local trauma during dressing changes.
- Prepare the periwound with skin barrier wipes that form a protective film over the periwound skin to reduce friction during removal of tapes and films.
Maintenance of skin integrity on the rest of the leg
- For healable AUs, humectants and/or emollients on desquamated areas in the periwound can help minimize skin breakdowns. Do not apply directly on the wound.
- For non-healable AUs (due to inadequate perfusion), guidelines recommended that all sources of moisture, such as foot soaks, creams and ointments be avoided to reduce risk of infection.[34][35]
Moisture management and dressing selection
Selection of primary and secondary dressings should follow established wound bed preparation principles.[6][3] For customized, wound-specific recommendations, use Wound Prep and Dress Tool. For practical information on dressing indications, contraindications, application, Medicare coverage and brands see "Dressing Essentials" and "Dressing Brands Quick Reference". General recommendations and evidence regarding dressings for AUs are listed below.
Moisture management
- For patients with AUs with arterial supply that is unknown and cannot be immediately determined, a non-healable wound program is recommended until arterial assessments are performed.[3]
- 1CFor non-infected healable AUs with adequate perfusion to promote healing, or after successful revascularization, we recommend clinicians apply a non-adherent dressing that will maintain a moist wound bed, protect periwound skin, and allow frequent visualization of the wound (Grade 1C).[8][24]
-
- Rationale: Several experimental studies support the hypothesis that a moist wound bed increases wound healing when compared to a dry wound bed, by facilitating cell migration and matrix formation.[36][37]
- However, AUs treated with moisture-retentive dressing should be carefully monitored for signs of infection.[2]
- For non-infected healable AUs without sufficient blood flow to heal (e.g., pending revascularization), moist wound healing and occlusive dressings are not recommended due to the potential of bacterial growth and infection.[38] For those AUs, dressings that provide good ventilation and permit frequent wound inspection are indicated.[8][24]
- For infected AUs, antimicrobial dressings and systemic antibiotics are recommended. See section ‘Treat the cause - Infection Control’ above.
- For non-healable/maintenance AUs or for AUs with dry gangrene or black stable eschar, if exudate is minimal or absent, guidelines suggest daily painting with povidone-iodine (10% PVP-I) and covering with a gauze to maintain a dry environment.[2] If exudate management is needed, non-adherent dressings may be applied.[24]
Dressing selection
- 2CFor healable AUs, taking into consideration Medicare coverage, costs and wound characteristics, we suggest clinicians initiate treatment with one of the primary dressings below (Grade 2C)
-
-
- For full-thickness wounds with high or heavy exudate: composite, specialty absorptive, alginate, fiber gelling dressing (hydrofiber)
- For full-thickness wounds with moderate levels of exudate: composite dressings, specialty absorptive, foam dressings
- For wounds with light levels of exudate: non-adherent dressing, foam dressings
- For wounds with minimal levels of exudate: non-adherent dressings, foam dressings
- For dry gangrene and stable black eschar: povidone-iodine (10% PVP-I)
- For infected wounds: antimicrobial dressings.
- Rationale: Currently, there is insufficient evidence to determine whether the choice of topical agent or dressing affects the healing of AUs. [39][24][3] Existing evidence is of low certainty (evidence level C) due to unclear or high risk of bias of the available studies. [39]
- Use of resources: With respect to cost, it is important that clinicians consider not only the cost of dressings when selecting dressings, but also cost of other resources needed to utilize each type of dressing.
A cheaper dressing that requires multiple dressing changes by clinicians will result in higher total costs compared to a more expensive dressing that requires less frequent dressing changes or does not require trained personnel for application. [40][41]
-
Wound characteristics: characteristics such as wound bed, depth, exudate should be considered when choosing dressings for AUs. Consideration should be made to change a product if an AU does not show signs of improvement after a couple of weeks. Adverse effects such as infection, or further loss of tissue should prompt a change in wound dressing as well. When selecting dressings for AUs, increased susceptibility to infection due to decreased immune response should be taken into account.
Hydrogels and occlusive dressings such as hydrocolloids can exacerbate clinically unsuspected (occult) infection. Poor hygiene also contributes to increasing infection rates.[42] For customized, wound-specific recommendations, use the Wound Prep and Dress Tool.
For practical information on dressing indications, contraindications, application, Medicare coverage and brands see topics "Dressing Essentials" and "Dressing Brands Quick Reference"
Plan Reassessment
For patients with minor tissue loss or infection and mild or moderate ischemia, conservative standard of care is indicated as the initial therapy. In those cases, if the AU does not show at least 50% decrease in size after 4 weeks of treatment with standard of care therapy should be reassessed for revascularization.[1][9][10][11][5] For management of patients with severe ischemia, or patients with either advanced tissue loss or infection and moderate ischemia, see section 'Management of arterial ulcers by healability and limb severity' above as well as topic "Arterial Ulcer - Surgical Treatment".
For details on standard therapy, see sections 'Treat the Cause', 'Address Patient Concerns' and 'Local Wound Care' above.
Re-evaluation of the patient and ulcer should be performed before use of adjuvant therapies.
Re-evaluation should include assessment of adequate interventions, and consideration of differential diagnoses. A checklist such as the one shown in Table 3 can be useful in reassessing plan of care:
Table 3. Checklist for reassessment of AU treatment plan
Focus on evaluating:
|
- Differential diagnoses
- Factors mitigating healing
- Comorbidities (e.g., uncontrolled diabetes, malnutrition, immunossuppression)
- Medications (e.g, steroids, immunosuppressants)
- Lifestyle (e.g., smoking)
- Blood supply to the ulcer(s)
- Barriers to adherence to treatment
- Offloading/ edema control effectiveness
- Presence of infection
- Ulcer moisture balance/ exudate control
- Need for vascular interventions
|
Then if appropriate consider:
|
- Biopsy or swab with validated method such as Levine technique to rule out infection/ osteomyelitis; initial biofluorescent scan if available
- Refer to infectious disease specialist if needed
- Biopsy to rule out malignancy, vasculitis, atypical ulcers
- Order or review ABI/ toe pressure/ Doppler waveform/ TcpO2 study, vascular imaging
- Order or review laboratory tests (e.g. complete metabolic panel, lipid panel, HbA1c)
- Consults/referrals:
- Vascular specialist, orthotist, podiatrist, infectious disease, behavioral medicine, hyperbaric oxygen therapy
|
Vascular Surgical Interventions
Lower extremity revascularization is one of the mainstays in treatment of AUs. For indications and perioperative care of vascular surgical interventions for AUs (e.g. lower extremity revascularization or lower limb amputation), see topic "Arterial Ulcer - Surgical Treatment" and section 'Indications for Surgical Revascularization' in the topic "Diabetic Foot Ulcer Associated with Ischemia - Management". For patients who are not candidates for revascularization, see section 'Non-revascularization Treatment of the Limb' below.
Adjunctive Therapy
Adjunctive therapies to promote AU healing should only be considered for healable AUs and if the healable AU does not show signs of improvement within 4 weeks of comprehensive care as described in this topic or if the adjunctive therapy is combined with revascularization. Adjunctive therapies do not correct the underlying vascular disease and are not a replacement for revascularization. Patient and ulcer should be re-evaluated prior to initiating adjunctive therapy. (See 'Plan Reassessment' above)
Wound Coverage
- For patients with AU who have undergone successful revascularization, clinicians might opt to provide wound coverage with autografts or allografts to accelerate wound healing.[1][3] See topic "Cellular and/or Tissue Based Products"
NEGATIVE PRESSURE WOUND THERAPY (NPWT)
- 2CFor patients with healable AUs without significant necrosis, clinicians might opt for adjunctive NPWT at lower pressures to promote healing (Grade 2C).
-
- Rationale: currently there is lack of strong evidence supporting use of NPWT to promote healing of AU.[43] Guidelines recognize NPWT may have a role as an adjuvant agent for AUs, but further study is required.[24][2] NPWT has been found to improve blood flow perfusion by enhancing vessel maturation and increasing the number of pericytes.[44]
However, there are concerns that NPWT can worsen necrosis in ischemic wounds.[45] While NPWT at higher pressures may actually impair wound healing when ischemia is present, NPWT at lower pressures (i.e. -75 mmHg of pressure) has been reported to be safely employed for treatment of AU patients.[46] Duration of treatment is determined by frequent wound surveillance. Patients should be selected on a case-by-case basis and NPWT should be discontinued at the first sign of necrosis.[46]
Noncontact low frequency ultrasound
- 2CFor patients with healable AU, clinicians might opt for noncontact low-frequency ultrasound as an adjunctive therapy to promote wound healing.(Grade 2C)
-
- Rationale: evidence is not strong enough to support routine use of low-frequency ultrasound (e.g. MIST) for AUs. A small RCT (n=35) demonstrated that this intervention may provide some evidence of benefit in AUs compared to standard care, however further studies are needed.[2][47]
Biophysical Interventions
Hyperbaric oxygen therapy
- 1BFor patients with PAD and DFU classified as Wagner 3 or higher, which failed to respond to standard therapy administered for at least 30 days, we recommend HBO therapy as adjunctive therapy to promote healing and decrease chances of amputation (Grade 1B).
- 2BFor other patients with PAD and DFUs that failed to respond to at least 30 days of standard therapy and have demonstrated good transcutaneous oxygen values response to 100% oxygen, clinicians might consider HBO therapy to promote DFU healing and decrease chances of amputation (Grade 2B).
-
- Rationale: Studies are required to determine whether these results can be generalized to pure arterial ulcers without the neuropathic component. In practice, if the patient is not a revascularization candidate or failed revascularization, amputation is the most likely intervention. For these patients, as long as they have a Wagner 3 DFU, an HBOT trial (10-15 sessions) may be offered.
If the ulcer shows signs of improvement, HBOT could be continued until at least 30 sessions. Otherwise, TcPO2 studies are helpful in determining the amputation level.
- For details, see topics " Diabetic Foot Ulcer - Hyperbaric Oxygen Therapy" and "Diabetic Foot Ulcer - Treatment".
Non-revascularization Treatment of the Limb
For patients who are not candidates for revascularization, clinicians might opt for non-revascularization treatments of the limb. These treatments are mostly unsupported by evidence and should be considered alternatives only on an individual basis and after careful consideration of benefits, risks and goals of care. Interventions include spinal cord stimulation, lumbar sympathectomy, intermittent pneumatic compression, and pharmacotherapy.
Spinal cord stimulation
- 2BFor carefully selected patients (e.g., with rest pain, minor tissue loss) in whom revascularization is not possible, clinicians might opt for spinal cord stimulation (SCS) to reduce the risk of amputation and decrease pain (Grade 2B).[1]
-
- Rationale: Spinal cord stimulation (SCS), originally used to treat chronic pain, may be used to stimulate sensory fibers, leading to vasodilation and better tissue perfusion. A Cochrane systematic review concluded that SCS offers a modest positive effect on pain relief and an 11% reduction in the amputation rate compared with conservative management after 1 year, despite being more expensive than the latter.[1][48]
Lumbar sympathectomy
- 2CFor patients with CLTI in whom revascularization is not possible, guidelines suggest against lumbar sympathectomy as an attempt to save the limb (Grade 2C).[1] However, lumbar sympathectomy (LS) may be an option to promote symptom relief for these patients. [1][49]
-
- Rationale: In LS, the lumbar sympathetic ganglia is denervated either laparoscopically or through percutaneous chemical blockade. LS increases blood flow to the lower limb, which can improve tissue oxygenation, decrease tissue damage and pain. Overall, data are limited, but there is no evidence to suggest that LS reduces the risk of major amputation in patients with CLTI. [1]
Intermittent Pneumatic Compression
- 2BFor carefully selected patients (e.g., patients with rest pain, minor tissue loss) in whom revascularization is not possible, clinicians might opt for Intermittent Pneumatic Compression (IPC) therapy (Grade 2B).
-
- Rationale: IPC promotes increase of arterial blood flow to the distal limbs, and stimulates growth of collateral artery.[1][50] While there have been no high quality studies (i.e. randomized controlled trials) analyzing IPC for treatment of AU, a systematic review of existing studies found that IPC may be associated with improved limb salvage, wound healing, and pain management as well as with a low risk of complications.[1][50]
- Coverage: for this indication, IPC is often not covered by Medicare or commercial insurance
Pharmacotherapy
Prostanoids
- 2BFor patients with CLTI, guidelines suggest against prostanoids for limb salvage (Grade 2B).[1]
- 2BFor carefully selected patients (e.g., patients with rest pain, minor tissue loss) in whom revascularization is not possible, clinicians might opt for prostanoids (Grade 2B).
-
- Rationale: Prostanoids act by inhibiting the adhesion and aggregation of platelets and by promoting vasodilation.[1]
- There is strong evidence that the use of prostanoids does not reduce the risk of amputation in CLTI patients in whom revascularization is not possible. [1][51]
A Cochrane systematic review showed that compared with placebo, prostanoids appeared to have some efficacy for treating rest pain (RR, 1.30; 95% CI 1.06 to 1.59) and ulcer healing (RR, 1.24; 95% CI 1.04 to 1.48).[1][51] In clinical practice, it appears that iloprost, a type of prostanoid, benefits approximately 40% of carefully selected patients in whom revascularization is not possible.[1]
Vasoactive drugs
- 1CFor patients in whom revascularization is not possible, guidelines recommend against use of vasoactive drugs or defibrinating agents (ancrod) (Grade 1C)
-
- Rationale: There is currently insufficient evidence to support the use of the following drugs in the treatment of CLTI:
-
- Vasoactive drugs such as naftidrofuryl [52], pentoxifylline [52], or cilostazol [1]
- Vasodilators [53]
- Defibrinating agents (ancrod) [54]
Experimental Interventions - Biologic and Regenerative Medicine Approaches
Biologic or regenerative medicine approaches include gene therapy and cellular therapy. These are promising interventions that offer the potential to promote wound healing and to prevent limb amputation in CLTI patients who are not candidates for revascularization.[1]
To date, no phase 3 trial has shown gene therapy and cellular therapy to be effective. However, there are multiple phase 3 clinical trials in progress, and if any of these therapies are proven effective, there could be a dramatic change in how patients with CLTI and AU are cared for in the future. Until further evidence is available, these therapies are considered investigational.
PREVENTION
- Refer to section 'Treat the cause and co-factors impeding healing' above.
PATIENT EDUCATION - FOR CLINICIANS
- Hospital discharge instructions for patients with PAD include lifestyle modifications; risk reduction therapies (e.g. antiplatelet, statins, and blood pressure management); and knowing symptoms of disease. [55]
- See patient education handout ""Patient Education - Arterial Ulcer".
APPENDIX
Summary of Evidence (SOE)
Negative pressure wound therapy
(back to text)
Guidelines:
- The 2014 Wound Healing Society (WHS) and the 2014 Wound, Ostomy, Continence Nursing Society (WOCN) guidelines support use of negative pressure wound therapy (NPTW) to promote wound healing, although the levels of evidence assigned by these societies differed from each other, possibly due to different evidence grading methodologies and different studies from which evidence was drawn (see table below) [2][24]
| Intervention for AU | WHS | WOCN |
Topical negative pressure wound therapy
| Level III | Level II (for wounds with infected vascular grafts) |
Hyperbaric oxygen therapy
(back to text)
Systematic reviews
- A 2020 systematic review by Brouwer et al. included 11 studies (n=729) that evaluated use of adjunctive HBOT in the treatment of diabetic foot ulcers with arterial insufficiency. Meta-analysis showed a significantly fewer major amputations in the HBOT group (10.7% vs 26.0%; P = .002). No difference was found for minor amputations (risk difference, 8%; 95% CI, -13 to 30; P = .46). Three studies reporting on complete wound healing showed contrasting results. No significant difference was found for mortality or amputation-free survival, complete ulcer healing, and mortality. Authors concluded that current evidence shows that adjuvant HBOT improves major amputation rate, but not wound healing, in patients with DFUs and PAD. Given the wide range of patients included in the trials, better patient selection may help define which patients with DFUs and PAD benefit most from HBOT as standard adjunctive treatment.[56]
Clinical guidelines
- The 2014 Wound Healing Society (WHS) and the 2014 Wound, Ostomy, Continence Nursing Society (WOCN) and the 2019 Society for Vascular Surgery, European Society for Vascular Surgery, and World Federation of Vascular Societies combined guidelines support use of adjunct HBOT to promote wound healing in patients with nonreconstructable anatomy or whose ulcer is not healing despite revascularization. The levels of evidence assigned by these societies differed from each other, possibly due to different evidence grading methodologies and different studies from which evidence was drawn (see table below) [2][24][1]
| Intervention for AU | WHS | WOCN | SVS |
In patients with nonreconstructable anatomy or whose ulcer is not healing despite revascularization, hyperbaric oxygen therapy (HBOT) should be considered as an adjuvant therapy.
| Diabetic ischemic ulcers—Level IA; nondiabetic ischemic ulcers—Level IIB)
| Level II | Does not grade the recommendation, but states that "Overall, whereas controversy remains, there may be a role for the use of HBOT to accelerate ulcer healing in diabetic patients with nonhealing neuropathic ulcers and low-grade ischemia who have failed to respond to conventional wound care." |