ABSTRACT
Wound care clinicians often face challenging ulcers that have been previously treated with little or no success by other healthcare providers. Some of these ulcers are related to cutaneous vasculitis. This topic provides an updated, summarized review on assessment and management of this often misdiagnosed condition. For a case study on how an atypical lower extremity ulcer was diagnosed as new-onset cutaneous vasculitis at a wound care clinic, see topic "Case: New-onset cutaneous vasculitis". For a list of other types of inflammatory ulcers, see topic "Inflammatory Ulcers".
Vasculitis of the skin (cutaneous vasculitis) includes several inflammatory disorders that compromise the cutaneous vascular system (i.e. arterioles, capillaries, postcapillary venules), and lead to cutaneous changes and ulcers. The 2012 revised International Chapel Hill Consensus Conference Nomenclature of Vasculitides and its updated dermatologic addendum classified vasculitic disorders and identified which of the variants have cutaneous manifestations - those are collectively known as "Cutaneous Vasculitis". See Table 1.
Assessment: Since cutaneous vasculitis can be secondary to drugs (including recreational), infections, sepsis, autoimmune disorders, etc, it is important to inquiry about new drugs, infections and comorbidities as part of the initial evaluation. The possibility of associated systemic vasculitis needs to be throughly assessed. Findings upon physical examination include palpable purpuras, ecchymosis, hemorrhagic bullas, ulcers, etc. Skin biopsy is an important element in confirming diagnosis. See sections History and Physical Exam, Diagnosis (biopsy and laboratory tests), Differential Diagnosis
Treatment: Once systemic involvement has been excluded, the treatment of cutaneous vasculitis should be focused on symptom management (e.g., use of topical or oral corticosteroids) and elimination of identifiable triggers. Local wound care should follow established principles of wound bed preparation. See sections
Treat the cause,
Provide effective wound care,
Adjunctive therapy.
INTRODUCTION
Background
Definition:
Vasculitis of the skin (cutaneous vasculitis) includes several inflammatory disorders that compromise the cutaneous vascular system (i.e. arterioles, capillaries, postcapillary venules), and lead to cutaneous changes.[1]
Epidemiology
Approximately 3% to 5% of skin ulcers may be caused by a vasculitic disorder.[1]
Pathophysiology
Cutaneous vasculitis (CV) results from vessel damage mediated by an immunological process that causes inflammation and destruction of both the vessels and the perivascular tissue.[1] The injury of cutaneous microvessels may result in impairment of blood flow and consequent focal ischemia and formation of skin ulcers. The ulcers are often multiple and localized on the lower leg and foot where the microcirculatory anatomy and rheologic dynamics are predisposing factors.[1]
Classification/ nomenclature:
According to the 2012 revised International Chapel Hill Consensus Conference Nomenclature of Vasculitides (CHCC2012) and its updated dermatologic addendum, cutaneous vasculitis can present in 3 main forms [2][3]:
1. A cutaneous component of systemic vasculitides (e.g., cutaneous manifestations of IgA vasculitis):
- Systemic vasculitis is a vasculitis that is present in at least one organ in addition to skin.
2. A skin-limited or skin-dominant expression or variant of a systemic vasculitis (e.g., skin-limited IgA vasculitis);
- Skin-dominant forms may develop into a full systemic vasculitis
3. A single-organ vasculitis (SOV) of the skin that differs from recognized systemic vasculitides with regard to clinical, laboratory, and pathologic features (e.g., nodular vasculitis).
- SOV does not develop into a full systemic vasculitis
Skin-limited vasculitis or cutaneous SOV is a diagnosis of exclusion and, there must be no detectable involvement of another, noncutaneous organ by vasculitis.[3]
The consensus classified vasculitic disorders and identified which of the variants have cutaneous manifestations - those are collectively known as "Cutaneous Vasculitis". See Table 1 below.
Updated classification of vasculitis and skin involvement status by vasculitis category and disease
|
Note: Diseases in purple may have a cutaneous component of systemic vasculitis or be skin-limited/ skin-dominant. Diseases in green are skin-limited only. Others do not typically have cutaneous manifestations.
Large vessel vasculitis - Temporal arteritis
- Takayasu arteritis
Medium vessel vasculitis - Polyarteritis nodosa
- Kawasaki disease
Small vessel vasculitis - Immunecomplex-mediated
- Anti-glomerular basement membrane disease (Goodpasture's Disease)
- Cryoglobulinemic vasculitis
- IgA vasculitis (Henoch-Schönlein purpura)
- Urticarial vasculitis
- ANCA-associated
- Granulomatosis with polyangiitis (Wegener)
- Eosinophilic granulomatosis with polyangiitis (Churg-Strauss)
- Microscopic polyangiitis
Variable vessel vasculitis - Behçet's disease
- Cogan's syndrome
Vasculitis associated with systemic disease - Systemic lupus erythematosus (SLE), rheumatoid arthritis, sarcoidosis, etc.
Vasculitis associated with probable etiology - Drugs, infections, sepsis, autoimmune diseases, etc.
Cutaneous single-organ vasculitis (SOV, not originally included in CHCC2012) - IgM/IgG vasculitis
- Nodular vasculitis (erythema induratum of Bazin)
- Erythema elevatum et diutinum
- Hypergammaglobulinemic macular vasculitis
- Normocomplementemic urticarial vasculitis
|
ASSESSMENT
History
Cutaneous vasculitis can present together with a series of generally non-specific signs and symptoms. Since cutaneous vasculitis can be secondary to drugs (including recreational), infections, sepsis, autoimmune disorders, etc, it is important to inquiry about new drugs, infections and comorbidities as part of the initial evaluation. The possibility of associated systemic vasculitis needs to be throughly assessed. A comprehensive history should be obtained, including [1][4]:
- Onset of the vasculitic lesions (drug-induced vasculitis often occurs within 10 days from introduction of the new medication)
- Symptoms that may indicate systemic vasculitis:
- General: fatigue, fever, night sweats, unexpected weight loss, edema of lower limbs
- Pulmonary: chest pain, dyspnea, cough or hemoptysis, new onset of asthma
- Gastro-intestinal/ Genito-urinary: abdominal pain and melena, associated to signs of nephropathy may indicate IgA vasculitis. Signs/symptoms of hepatitis B and C, as those can induce vasculitis.
- Neurological: Neurologic manifestations: peripheral neuropathies
- Rheumatological/ musculoskeletal: persistent polyarthritis, SLE, rheumatoid arthritis, other connective tissue disorders
Physical Exam
Cutaneous manifestations of vasculitis include [1][2][3][4]:
- Palpable purpura: most common sign among several cutaneous vasculitis. Lesions begin as erythematous maculae that become purpuric papule sometimes confluent, that evolve to plaque, nodule and ulcer. Usually purpura have a diameter of less than 1 cm.
- Other types of changes include ecchymosis, hemorrhagic bullas, livedo reticularis
- Ulcers may be the first presentation or appear following other skin changes. Ulcers are usually small, multiple, and tend to coalesce in greater polycyclic lesions. They mainly appear at the lower limbs at various levels, with particular incidence in the lower half of the leg and, rarely, the fingers of the hands.

Fig. 1. Palpable purpura on leg

Fig. 2. Livedo reticularis (due to cryoglobulinemia)
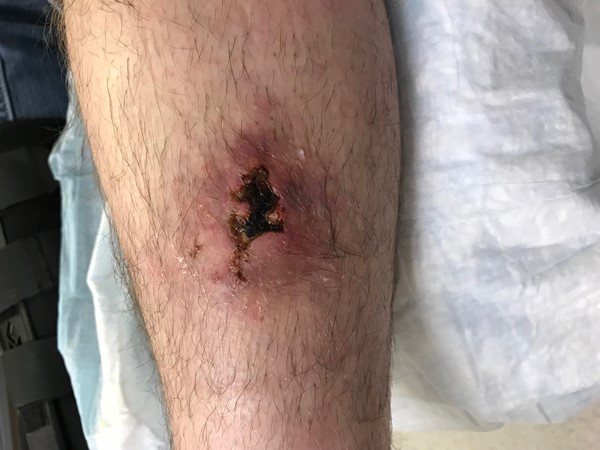
Fig. 3. Vasculitic ulcer on leg
Diagnosis
Biopsy
Biopsies (H&E and direct immunofluorescence) are important to confirm the diagnosis and identify patients at higher risk of systemic complications. The specimen should be taken at the active edge of the lesion or in the periwound area when new lesions tend to develop.[1][3]
- H&E: Ideally obtained from a lesion that is between 24 and 48 hours old, so as to increase chances of detecting leukocytoclastic immune complex vasculitis (LCV). The histopathologic features of cutaneous vasculitis are influenced by treatment and duration of time since onset.[3]
- Direct immunofluorescence (DI): Ideally obtained from a lesion that is less than 24 hours old. Immunofluorescence analysis for demonstration of immunoreactants in dermal vessels ideally requires biopsy of an early or histamine-induced lesion, because immunoglobulins may disappear over time.[3]
If necrotizing or leukocytoclastic vasculitis is confirmed histologically, the possibility of systemic vasculitis, an infection, medication, or a systemic disease such as systemic lupus erythematosus must be searched before reaching definitive diagnosis.[5]
Laboratory tests
Besides histological examination, laboratory tests should be ordered when cutaneous vasculitis is suspected. Initial tests include:
- Erythrocyte sedimentation rate (ESR), C reactive protein (CRP)
- Creatinine, urea blood test
- GOT, GPT, alkaline phosphatase, γGT PT, PPT
- Antinuclear antibody
- Rheuma-test
- Urinalysis
- Fecal research of occult blood
- Antibodies anti-hepatitis B virus; antibodies anti-hepatitis C
Other tests typically ordered by rheumatologists or other vasculitis specialists include:
- Hemochrome
- Fibrinogen
- Protein electrophoresis
- C3, C4, CH50
- Extractable nuclear antigens antibodies (anti-ENA)
- Antineutrophil cytoplasmic antibodies (c, p-ANCA)
- Cryoglobulins
Differential Diagnosis
Besides the vasculitis variants (Table 1), differential diagnosis include cellulitis, arthropod bites, macular purpura owing to trauma, skin fragility, or anticoagulation, platelet dysfunction or deficiency, pigmented purpuric dermatosis, cholesterol emboli, septic emboli, livedoid vasculopathy, etc.
TREATMENT
Treat the cause
- Once systemic involvement has been excluded, the treatment of cutaneous vasculitis should be focused on symptom management and elimination of identifiable triggers.
- To decrease stasis-related immune complex deposition and accelerate healing of ulcers the following measures are suggested: avoidance of prolonged standing, rest, limb elevation, use of compression stockings or compression bandages if no severe peripheral artery disease is present.[1][4]
- For vasculitic inflammatory lesions, topical steroids may relieve itch or burning but will not prevent new lesions from developing. Use of tacrolimus ointment 0.1% has been reported to help heal refractory vasculitic ulcers.[1]
- If vasculitic ulcers are present: may initiate prednisone, with initial doses of 0.5 to 1 mg/kg per day. Dose should be tapered slowly to prevent rebound. For refractory cases, treatment options include colchicine (0.6 mg 2–3 times per day, if tolerated) and dapsone (50–200 mg/d).[4]
Address patient's concerns
- Lesions may be very painful. The World Health Organization (WHO) Pain Ladder for cancer patients, with modifications for wound care may be used. Benefits and harms of each step should be considered. In summary [6]:
- Step 1: A non-opioid analgesic (e.g., NSAID) with or without an analgesic adjuvant. Adjuvants include tricyclic antidepressants (e.g., nortriptyline starting at 10-30 mg at night), anticonvulsants (e.g., gabapentin), antihistamines, benzodiazepines, steroids, and phenothiazines.
- Step 2: If pain is not controlled: Continue the initial medication and add an opioid, such as codeine or tramadol, and an adjuvant
- Step 3: If pain is not controlled: Discontinue second step medications and initiate a more potent oral narcotic
Provide effective wound care
- Ulcers due to vasculitis should follow the same principles of wound bed preparation like other ulcers.[1] Appropriate local wound care should be implemented (i.e. cleansing, debridement of non-viable tissue, infection and bioburden control, moisture management). For customized, wound-specific recommendations, use Wound Prep and Dress Tool.
- As for debridement, surgical debridement should be done with care on patients with active vasculitis, due to risk of “pathergy”, a phenomenon that usually consists in the formation of severe necrotic or undermined lesions in the areas that have been debrided.[1]
Prognosis
Overall, prognosis is favorable, particularly in the absence of systemic disease.[4]
Adjunctive therapy
- For nonhealing vasculitic ulcers, improved outcomes with iloprost (a stable prostacyclin analogue) have been reported.[7]
- For systemic vasculitis, corticosteroids in combination with cytotoxic drugs (most commonly cyclophosphamide) has been shown to improve prognosis. Rituximab has also been used with good results in many cases of systemic vasculitis.[8][1]