This topic provides a review on the available knowledge on cutaneous manifestations associated with COVID-19, based on literature review and on data published by the international registry from the American Academy of Dermatology and International League of Dermatological Societies.
The incidence of cutaneous manifestation among patients with COVID-19 remains unclear, with studies reporting 0.2% to 20%.[1] Literature has reported a wide range of cutaneous manifestations in patients with COVID-19. While many of those manifestations are nonspecific and occur during or after other COVID-19 signs, recognizing these manifestations may pose an opportunity to improve diagnosis and management. This topic is based on the available literature, which still consists primarily of care reports, registries and small case series (low certainty evidence).[1][2]
CUTANEOUS MANIFESTATIONS ASSOCIATED WITH COVID-19
Groups and types of cutaneous manifestations
Based on the analysis of hundreds of patients, a framework explaining 2 mechanistic patterns that result in cutaneous manifestations of COVID-19 has been proposed by Suchonwanit et al [3] and supported by many [1][2]:
- Inflammatory or exanthemous patterns: lesions in this group have clinical features similar to viral exanthems. This group includes the following main clinical patterns:
- Pernio (chilblain)-like acral lesions ("COVID toes")
- Morbilliform/ erythematous/ maculopapular rash
- Urticarial rash
- Papulovesicular exanthem
- Vasculopathic and vasculitic patterns: this group of lesions consists of cutaneous eruptions secondary to COVID-19 systemic consequences, especially vasculitis and thrombotic vasculopathy. Those include:
- Retiform purpura/ livedo racemosa/ necrotic vascular lesions
Pernio (chilblain)-like acral lesions have been reported to be associated with milder COVID-19 disease courses, whereas retiform purpura/ livedo racemosa/ necrotic vascular lesions have been associated with severe disease in critically ill patients.[1]
Most COVID-19 cutaneous manifestations occur after onset or at the same time as other COVID-19 symptoms. However, lesions may also present prior to other COVID-19 symptoms: the international registry from the American Academy of Dermatology and International League of Dermatological Societies reported a case series in that 12% of patients presented skin manifestations before other COVID-19 signs.[1]
Of note, patients with COVID-19 are more likely to present with adverse drug reactions and interactions due to their treatment, leading to secondary cutaneous reactions.[3]
Table 1 below summarizes characteristics of cutaneous manifestations in patients with COVID-19 by group and type of cutaneous manifestation. Pictures representing inflammatory or exanthemous patterns and vasculopathic or vasculitic patterns are shown on Table 2 and 3, respectively.
Table 1. Characteristics of cutaneous manifestations in patients with COVID-19 by group and type of cutaneous manifestation [1][2]
Inflammatory or exanthemous patterns
| Onset
| Characteristics
| Differential diagnosis
| Possible histopathological findings
|
Pernio (chilblain)-like acral lesions
| Mostly "after COVID-19 symptoms", followed by "before symptoms", and "at the same time as COVID-19 symptoms"
| - Associated with milder cases of COVID-19, often affects younger patients
- Feet (84%, "COVID toes") and hands (32%)
- The underlying cause of pernio-like lesions (per pathology findings) suggests a primary inflammatory process [1]
- May manifest asrythematous-violaceous or purpuric macules
- Often painful, pruritus may or may not be present
- Last approximately 2 weeks
| Perniosis, autoimmune connective tissue disease such as dermatomyositis, and systemic lupus erythematosus, acral livedo racemosa, retiform purpura, and acro-ischemia (skin manifestations of severe COVID-19). Pernio-like lesions are generally nonischemic, unlike retiform purpura and acral ischemia
| Vacuolar interface changes with associated necrotic keratinocytes, papillary dermal edema, superficial and deep dermal lymphocytic infiltrate, frequent vascular changes, dense perivascular and perieccrine sweat gland inflammation, predominance of CD3+/CD4+ T cells, and presence of CD303+ plasmacytoid dendritic cells and CD30+-activated cells in the dermal infiltrate. [4]
|
The term morbilliform refers to a rash that looks like measles, that is, macular lesions that are red and usually 2–10 mm in diameter but may be confluent in places." data-original-title="" title="" style="text-align: start;">Morbilliform/ erythematous/ maculopapular rash
| Mostly "after COVID-19 symptoms", followed by "at the same time", and "before COVID-19 symptoms"
| - Associated with moderate severity COVID-19
- Trunk and extremities
- Pruritus is common
| Cutaneous drug reaction, other viral rash | Diffuse vacuolar interface dermatitis, dyskeratotic keratinocytes predominantly localized to the basal layer, with lymphocyte exocytosis, superficial perivascular inflammation
|
Urticarial rash
| Mostly "after COVID-19 symptoms", followed by "at the same time", and "before COVID-19 symptoms"
| - Associated with moderate severity COVID-19
- Trunk and extremities
- Pruritus is common
| Cutaneous drug reactions, other viral rash
| Upper dermal edema, perivascular infiltrate of lymphocytes and some eosinophils
|
Papulovesicular exanthem
| Mostly "after COVID-19 symptoms", followed by "at the same time", and "before COVID-19 symptoms"
| - Associated with moderate severity COVID-19
- Trunk and extremities
- Pruritus is common
| Cutaneous drug reaction, other viral rash
| Superficial and deep perivascular dermatitis
|
Vasculopathic or vasculitic patterns
| Onset | Characteristics | Differential diagnosis | Possible histopathological findings
|
Retiform purpura is a specific morphology within the spectrum of reticulate eruptions of vascular origin. It develops when blood vessels serving the skin are compromised resulting in downstream cutaneous ischemia, purpura, and necrosis. Georgesen et al, 2020" data-original-title="" title="" style="text-align: start;">Retiform purpura/ Livedo racemosa is a cutaneous finding characterized by a persistent, erythematous or violaceous discoloration of the skin, in a broken, branched, discontinuous and irregular pattern, that can be either restricted to the limbs or be diffuse. It is usually the first sign of a systemic vascular disorder. Pincelli et al, 2020" style="outline: 0px; text-align: start;">livedo racemosa/ Livedo reticularis is a cutaneous physical sign characterized by transient or persistent, blotchy, reddish-blue to purple, net-like cyanotic pattern Sajjan VV et al, 2015" style="text-align: start;">livedo reticularis/ necrotic vascular lesions/ true acral ischemia
| Mostly "after COVID-19 symptoms", followed by "at the same time", and "before COVID-19 symptoms"
| - Associated with severe COVID-19
- Extremities and buttocks
- Often no pruritus, may be sometimes painful
- In darker skin: erythema may clinically manifest as subtler dark purple/brown hyperpigmentation
- Severe acro‐ischemia: finger or toe cyanosis, skin blisters and dry gangrene, resulting from a hypercoagulable status or confirmed disseminated intravascular coagulation [5]
- Platelet count, coagulation studies, and assessment of fibrin degradation products are helpful in assessing those patients
| Pernio (chilblain)-like acral lesions, pressure-induced necrosis, other types of vasculitis
| Noninflammatory to pauci-inflammatory thrombotic vasculopathy |
Table 2. Inflammatory or exanthemous patterns of COVID-19 skin manifestations
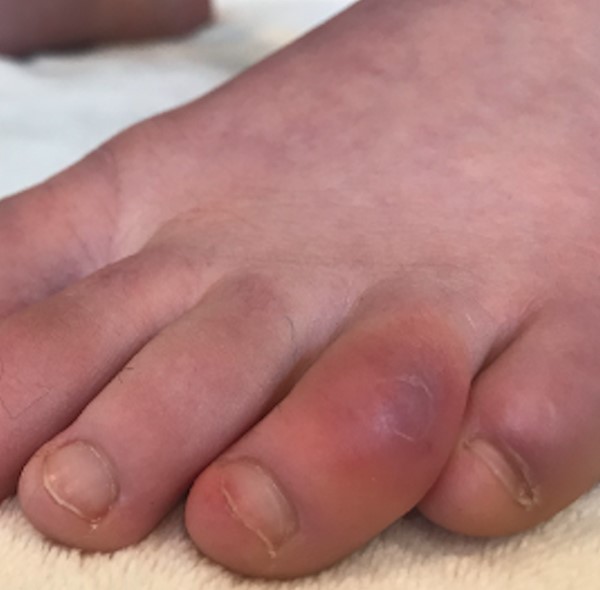 Fig.1. Pernio (chilblain)-like acral lesions ("COVID toes")
| 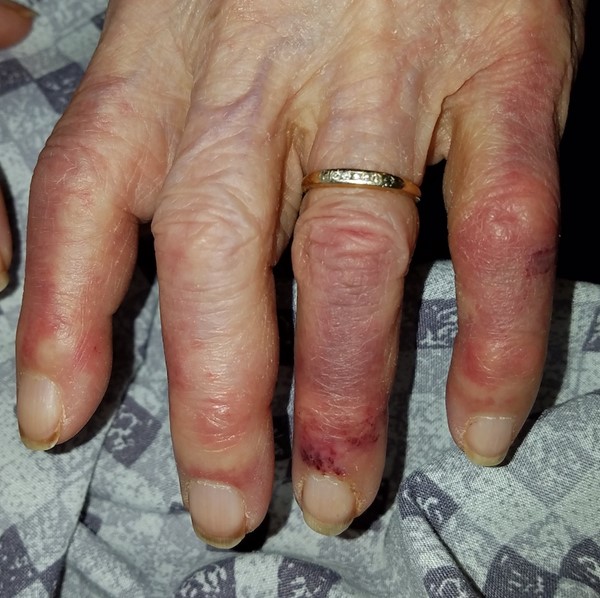
Fig.2. Pernio (chilblain)-like acral lesions (fingers)
| 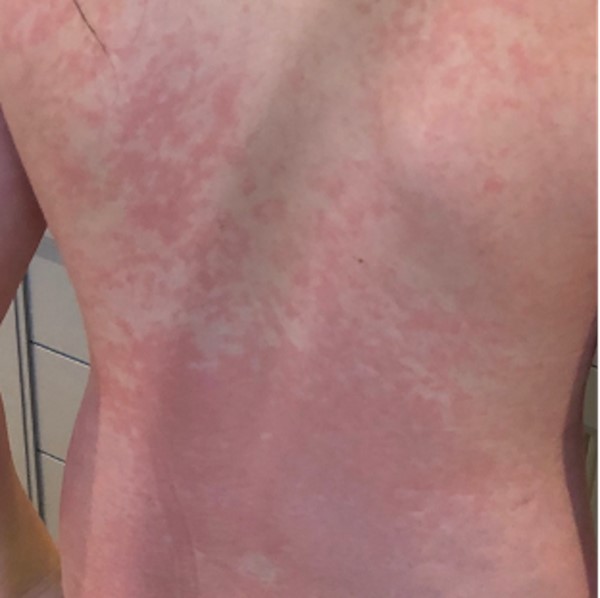 Fig. 3. Morbilliform rash on back |
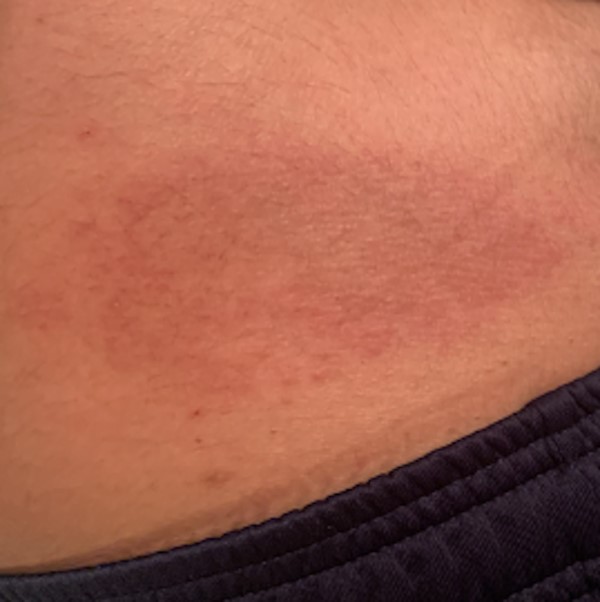
Fig. 4. Erythematous rash on abdomen | 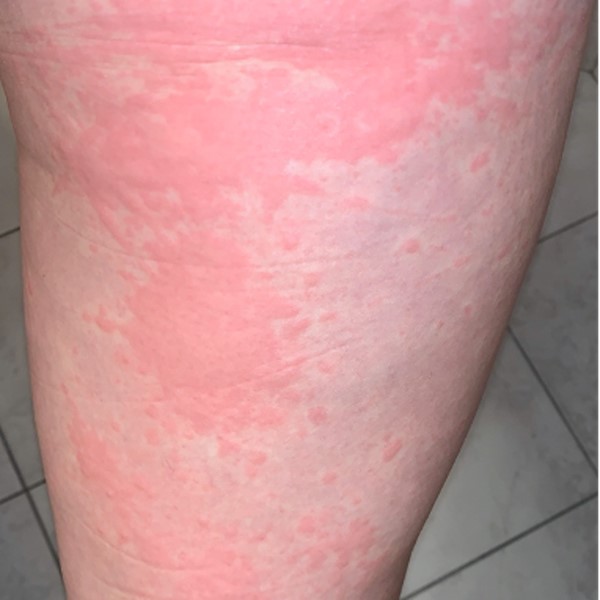
Fig. 5. Urticarial rash on posterior thigh | 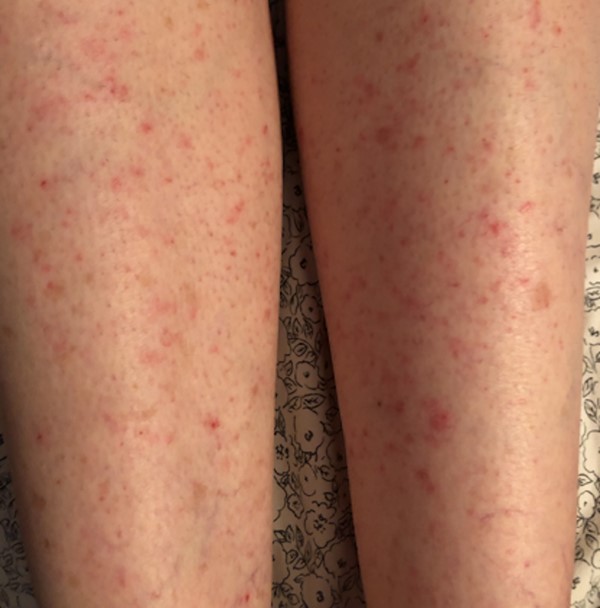
Fig. 6. Papulovesicular exanthem on legs |
Figures 1,3,4,5 and 6 (licensed under CC BY 4.0) [6]
Table 3. Vasculopathic or vasculitic patterns of COVID-19 skin manifestations
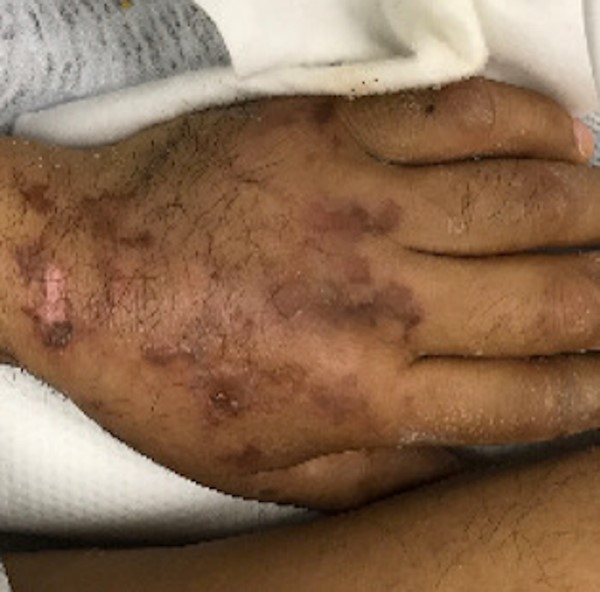
Fig. 7. Retiform purpura of the hand | 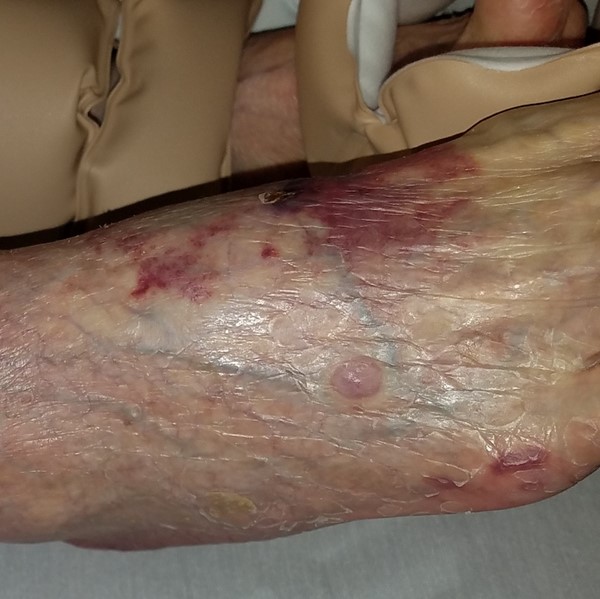
Fig. 8. Retiform purpura on dorsum of foot | 
Fig. 9. Livedo racemosa and retiform purpura |
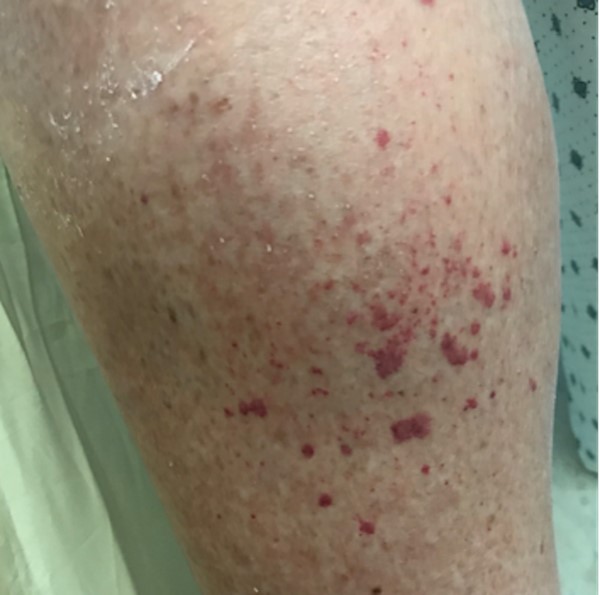
Fig. 10. Petechiae/purpura on calf | 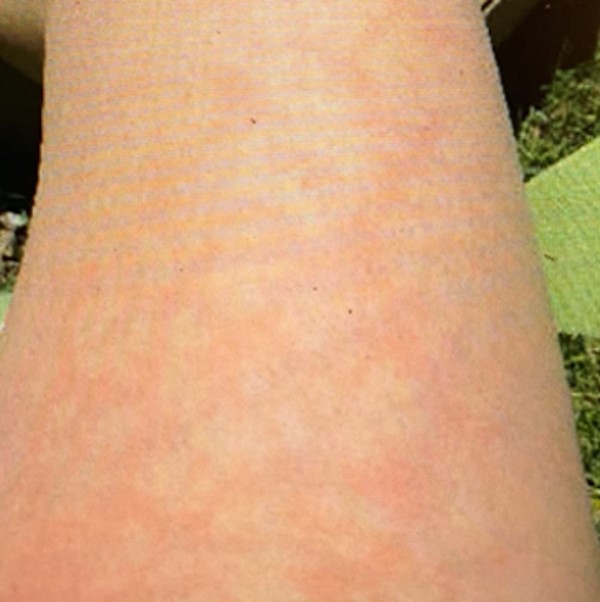
Fig. 11. Livedo reticularis | 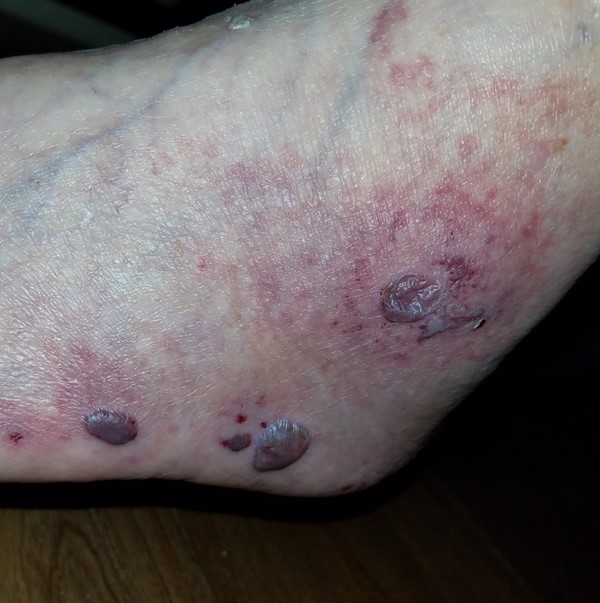
Fig. 12. Hemorrhagic bullae and vasculitis on foot |
Figures 7,9,10,11 (licensed under CC BY 4.0) [6]
Other case reports
- In May 2020, Robles et al reported a case series 41 patients with COVID-19 with chilblain-like lesions (erythematous or purplish papules and plaques, similar to chilblain lesions caused by cold). Lesions were seen on the feet alone (80%, including "COVID toes"), followed by hands and feet (10%), hands (7%) and ears (2%).
- A case reported by Joob and Wiwanitkit in May 2020 illustrated a case in which an afebrile patient with COVID-19 initially presented with a skin rash with petechiae that was misdiagnosed by dengue. Authors cautioned that there is a possibility that a patient with COVID-19 might initially present with a skin rash that can be misdiagnosed as another common disease.
- Magro et al reported in April 2020 5 severe COVID-19 cases, 3 of which had purpuric skin rash. Skin biopsy showed an extensive pattern of pauci-inflammatory vascular thrombosis with endothelial cell injury.
- A French observational study by Bouaziz et al published in April 2020 concluded that skin symptoms of COVID-19 may include erythematous rash, urticaria and chicken pox like lesions.
- In April 2020 Bellosta et al reported increased incidence of acute limb ischemia (ALI) among patients with COVID-19. Authors suggested that hypercoagulability in their patients were not related to well-known blood disorders, but that rather native arterial thrombosis may be triggered by COVID-19 infection.
- A case series by Recalcati published in March 2020 analyzed 88 patients with COVID-19 treated in Italy and found cutaneous manifestations in 18 patients (20.4%). Lesions were erythematous rash (14 patients), widespread urticaria (3 patients) and chickenpox-like vesicles (1 patient). Trunk was the main involved region. Given their transient nature, the author speculated that those skin manifestations are similar to cutaneousinvolvement occurring during common viral infections.
- Expert opinion published by Arora et al in March 2020 highlighted that patients with rheumatologic skin diseases (e.g. systemic lupus erythematosus, systemic sclerosis, mixed connective tissue disease and rheumatoid arthritis) may present with exacerbation of these conditions triggered by active COVID-19 disease.