Last updated on 3/13/24 | First published on 4/24/18 | Literature review current through Oct. 2024
[cite]
Authors:
Elaine Horibe Song MD, PhD, MBA,
Nataliya Lebedinskaya RN, BSN, CWOCN,
Topic editors:
Scott A. Robinson MD,
more...
Coauthor(s)
Elaine Horibe Song, MD, PhD, MBACo-Founder and Editor, Wound Reference, Inc;
Professor (Affiliate), Division of Plastic Surgery, Federal University of Sao Paulo;
Chair, Association for the Advancement of Wound Care;
Google Scholar Profile
Disclosures: Nothing to disclose
Nataliya Lebedinskaya, RN, BSN, CWOCN
Disclosures: Nothing to disclose
Editors
Scott A. Robinson, MD
Disclosures: Nothing to disclose
INTRODUCTION
Background
A pressure ulcer (PU), also known as pressure injury (PI), is localized damage to the skin and/or underlying soft tissue usually over a bony prominence or related to a medical or other device. Lesions occurs as a result of intense and/or prolonged pressure or pressure in combination with shear. The tolerance of soft tissue for pressure and shear may also be affected by microclimate, nutrition, perfusion, co-morbidities and condition of the soft tissue. Lesions may present as intact skin despite the presence of pressure-induced deep tissue damage, or as an open ulcer. [1][2] (Figure 1)
Guidelines, Quality Measures and resources for PU/PI prevention, assessment and management are listed below. For an introduction and assessment of PU/PI including epidemiology, risk factors, etiology, pathophysiology, history, physical examination, diagnosis, differential diagnoses, documentation and ICD-10 coding, see "Pressure Ulcers/Injuries - Introduction and Assessment". For PU/PI management, see " Pressure Ulcers/Injuries - Treatment". For PU/PI prevention, see "Pressure Ulcers/Injuries - Prevention". For best practices in care coordination, see "Pressure Ulcers/Injuries -Coordination of Care".
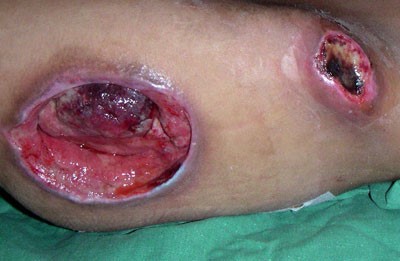
Figure 1. Pressure ulcers/ injuries (trochanter and iliac crest)
Terminology
In 2016 the National Pressure Injury Advisory Panel (NPIAP) updated the pressure ulcer staging system, including a shift in terminology from pressure ulcer to pressure injury. [2] These changes were made to more accurately describe pressure injuries to both intact and ulcerated skin. In the previous staging system Stage 1 and Deep Tissue Injury described injured intact skin, while the other stages described open ulcers. This led to confusion because the definitions for each of the stages referred to the injuries without actual ulcers as “pressure ulcers”.
Although the development of PU/PI staging systems is driven primarily by science, PU/PI staging in clinical practice tends to be driven more by regulatory and legal forces. [3] Some Federal documents (CMS) and quality measures are being updated to incorporate terminology updates. [4][5] As the new terminology may cause some short-term issues in regards to coding, payment, etc, we will follow the terminology used by CMS to ensure alignment with reimbursement and coding guidelines. It should be noted that the recommended change by NPIAP to PI does not represent a mandate. Thus, institutions must decide which term to use. [3]
Relevance
- In the United States only, approximately 3 million patients are affected by PU/PI, and each year 60 000 of them die from these ulcers. [6][7]
- PU/PI represent the second-most common hospital billing claim. Among Medicare beneficiaries, PU/PI add $43 000 to each hospital stay. [3]
- Despite the establishment and implementation of prevention guidelines, PU/PI continue to occur. PU/PI management may be hampered by variations in the descriptions of clinical stages of PU/PI, with poor reliability between observers.[3]
- In 2006 under the Hospital-Acquired Conditions (Present on Admission Indicator) program, PU/PI was identified by the Centers for Medicare and Medicaid Services (CMS) as one of the 14 hospital-acquired conditions (HACs) that are reasonably preventable using evidence-based guidelines.[8] Along the many recent CMS “value-based purchasing” initiatives, in 2008 CMS decided not to reimburse hospitals for Stage III and IV PU/PI and other preventable HACs, an effort that ties payment to performance. [9]
EVIDENCE-BASED CLINICAL GUIDELINES
Below is a list of the some of the most recent evidence-based guidelines on PU/PI:
| Evidence-based guideline, year |
Publishing Organization, country |
Links |
Comments |
WHS guidelines for the treatment of pressure ulcers-2023 update, 2024 [10]
| Wound Healing Society (WHS) | Guideline (Free) | Compendium of the evidence for the treatment of Pressure Ulcers published since the last update in 2015 and includes a new section based on changing demographics entitled 'Palliative wound care for seriously ill patients with pressure ulcers'.
|
Wound, pressure ulcer and burn guidelines - 2: Guidelines for the diagnosis and treatment of pressure ulcers, second edition, 2020
| The Japanese Society of Pressure Ulcers (JSPU)
| Guideline (Free) | Focus on management of pressure ulcers |
Prevention and Treatment of Pressure Ulcers: Clinical Practice Guidelines and Quick Reference Guide, 2019 [11]
| European Pressure Ulcer Advisory Panel, National Pressure Injury Advisory Panel and Pan Pacific Pressure Injury Alliance
| Clinical Practice Guidelines (For purchase) Quick reference guide (Free) | Updated version of the 2014 guideline. Only the Quick Reference guide is available free of charge. The authors note that it contains only excerpts and should be used in conjunction with the Clinical Practice Guidelines.
|
|
Guideline for Prevention and Management of Pressure Ulcers (Injuries), 2016 [12]
|
Wound, Ostomy and Continence Nurses Society (WOCN Society), USA |
Guideline (Purchase)
Summary (Free)
|
Updated version of the 2010 guideline. The updated document includes a summary of recommendations and an overview of the definition, background, significance, etiology, prevalence and incidence, classification system, as well as medical device-related pressure ulcers. As well as information for overall management goals, assessment and treatment strategies, preventative interventions |
The wound/burn guidelines - 2: Guidelines for the diagnosis and treatment for pressure ulcers, 2016 [13]
| Wound/Burn Guidelines Committee, Japan
| Guideline (Free) | Focuses on treatment, prevention, and care of pressure ulcer. |
Risk Assessment and Prevention of Pressure Ulcers: A Clinical Practice Guideline From the American College of Physicians, 2015 [14]
| American College of Physicians, USA
| Guideline (Free)
| Focus on comparative effectiveness of risk assessment scales and preventive interventions for pressure ulcers.
|
Wound healing society 2015 update on guidelines for pressure ulcers, 2015 [15]
| Wound Healing Society (WHS), USA
| Original guideline (2006) (Free) Guideline update (2015) (Free) | Includes clinical human and well‐controlled animal studies
|
Prevention and Treatment of Pressure Ulcers: Clinical Practice Guidelines and Quick Reference Guide, 2014 * [16]
| National Pressure Ulcer Advisory Panel (NPUAP), European Pressure Ulcer Advisory Panel (EPUAP), and Pan Pacific Pressure Injury Alliance (PPPIA), International
| Clinical Practice Guidelines (For purchase) Quick reference guide (Free) Support documentation(Free) | Only the Quick Reference guide is available free of charge. The authors note that it contains only excerpts and should be used in conjunction with the Clinical Practice Guidelines. Provides recommendations for risk assessment policy and practice, skin assessment, patient nutrition, patient repositioning techniques and practices, support surfaces. Includes some recommendations specific to patients in the operating room |
Pressure ulcers: prevention and management, 2014 [17]
| National Institute for Health and Care Excellence (United Kingdom)
| Guideline (Free)
| Focus on prevention and management
|
Pressure Ulcer Prevention, 2012 *[18]
| Hartford Institute for Geriatric Nursing, USA
| Book (for purchase)
| Prevention, assessment,management of PU/PI
|
Pressure Ulcer Guidelines, 2010 * [19]
| Association for the Advancement of Wound Care (AAWC), USA
| AAWC Pressure Ulcer Guidelines 8.11 (free) AAWC Pressure Ulcer Guideline Evidence Table 8.11(free) AAWC Pressure Ulcer Care Quick Reference Guide 9.11(free) AAWC Pressure Ulcer Guideline Algorithm Presentation 8.13 (free) AAWC Pressure Ulcer Guideline Checklist 7.13 (free) | Comprehensive guidelines include recommendations for patient assessment, risk factor assessment, and preventive care, including positioning, hydration, and nutrition.
|
* Selected evidence-based recommendations listed on CMS Report "Evidence-Based Guidelines for Selected Hospital-Acquired Conditions" [9]
QUALITY MEASURES
Relevant Quality Measures are listed below. For CMS MIPS measures, benchmarks are available on the CMS Quality Payment Program Measures Benchmarks.
| Setting |
CMS Program |
Developed by |
Measure ID |
Title |
Description |
| Post-acute |
Post-acute care Quality Reporting Programs (Home Health, Inpatient Rehabilitation Facility, Long-Term Care Hospital, Skilled Nursing Facility) (*) |
CMS and RTI International |
CMIT Measure ID: 121 |
Changes in Skin Integrity Post-Acute Care: Pressure Ulcer/Injury (data collection begun in 2018)
|
This cross-setting quality measure reports the percentage of patients/residents with Stage 2-4 pressure ulcers, or unstageable pressure ulcers due to slough/eschar, non-removable dressing/device, or deep tissue injury, that are new or worsened since admission. Measure follows updated PU/PI classification adopted by CMS as per recommendations of the National Pressure Injury Advisory Panel (NPIAP). It is the result of the standardization of NFQ0678 for implementation and use across health care settings. Publicly reported on LongTerm Care Hospital Compare and on Inpatient Rehabilitation Facility Compare
|
| Post-acute |
Post-acute care Quality Reporting Programs (Home Health, Inpatient Rehabilitation Facility, Long-Term Care Hospital, Skilled Nursing Facility) (*) |
CMS |
CMIT Measure ID: 521 |
Percent of Residents or Patients with Pressure Ulcers That Are New or Worsened (Short-Stay)
|
Percent of patients or short-stay residents with Stage 2-4 pressure ulcer(s) that are new or worsened since admission. For SNF/NH residents, this measure is restricted to the short-stay population defined as those who have accumulated 100 or fewer days in the SNF/NH as of the end of the measure time window. In IRFs, this measure is restricted to IRF Medicare (Part A and Medicare Advantage) patients. In LTCHs, this measure includes all patients. Note: NFQ0678 was replaced with "Changes in Skin Integrity Post-Acute Care: Pressure Ulcer/Injury"(*) |
| Post-acute | Nursing Home Quality Initiative
| CMS | CMIT Measure ID: 512
| Percent of High-Risk Residents With Pressure Ulcers (LS)
| This measure captures the percentage of long-stay, high-risk residents with Stage 2-I or unstageable pressure ulcers
|
| Hospital Inpatient |
Hospital-Acquired Condition Reduction Program (HACRP) (**)
|
Agency for Healthcare Research and Quality |
PSI 03 |
Patient Safety Indicator 03 (PSI 03) Pressure Ulcer Rate
|
Stage 3 or 4 (or unstageable) pressure ulcers (secondary diagnosis not present on admission) per 1,000 hospital discharges of surgical or medical patients ages 18 years and older. Excludes discharges with length-of-stay less than 3 days; with a principal diagnosis of stage 3 or 4 (or unstageable) pressure ulcer or deep tissue injury at the same anatomic site; with severe burns; or with exfoliative skin disorders; and obstetric discharges. Excludes numerator events with a secondary diagnosis code for deep tissue injury or unstageable pressure ulcer present on admission at the same anatomic site. Publicly reported on Hospital Compare
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| US Wound Registry | USWR22 | Patient Reported Measure: Patient Reported Nutritional Assessment in Patients with Wounds and Ulcers
| The percentage of patients aged 18 years and older with a diagnosis of a wound or ulcer of any type who self-report nutritional screening with a validated tool (such as the Self-MNA® by Nestlé) as well as food insecurity assessment, AND for whom the clinician provides and documents a follow up/ intervention plan within the 12-month reporting period.
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| CMS | MIPS 128 | Preventative Care and Screening: Body Mass Index (BMI) Screening and Follow-Up
| Percentage of patients aged 18 years and older with a BMI documented during the current encounter or during the previous twelve months AND with a BMI outside of normal parameters, a follow-up plan is documented during the encounter or during the previous twelve months of the current encounter
|
Outpatient
| Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| CMS | MIPS 155 | Falls: Plan of Care
| Percentage of patients aged 65 years and older with a history of falls that had a plan of care for falls documented within 12 months.
|
| Retired |
|
|
|
|
|
| Setting | CMS Program | Developed by | Measure ID | Title | Description |
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| US Wound Registry
| USWR23
| (RETIRED) Non Invasive Arterial Assessment of patients with lower extremity wounds or ulcers for determination of healing potential
| Percentage of patients aged 18 years or older with a non healing lower extremity wounds or ulcers that underwent a non-invasive arterial assessment once in a 12 month period, stratified by ABI, perfusion pressure, or oximetry. Data from the USWR indicates that fewer than 10% of patients with chronic non-healing leg ulcers undergo any type of vascular assessment (ABI, transcutaneous oximetry or skin perfusion pressure) even at hospital based outpatient wound centers.
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| US Wound Registry
| USWR24 | (RETIRED) Patient Reported Experience of Care: Wound Outcome
| All eligible patients with wounds or ulcers who completed of Wound Outcome Questionnaire who showed 10% improvement at discharge or transfer to another site of care during the 12 month reporting period
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| US Wound Registry
| USWR25 | (RETIRED) Outcome measure: Non-lower extremity Pressure Ulcer* (PU) Healing or Closure
| Percentage of Stage 2, 3, or 4 pressure ulcers among patients age 18 or older that have achieved healing or closure within 6 months, stratified by the Wound Healing Index. Healing or closure may occur by secondary intention or may be the result of surgical intervention (e.g. rotational flap or skin graft). According to the USWR, the most optimistic healing rate for pressure ulcers is likely 40% based on prospective trials data but could be 30% at 12 weeks based on real-world patient data. It is necessary to stratify pressure ulcers by risk category in order to establish benchmark healing rate data.
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (***)
| Medicare | MIPS 131 | (RETIRED) Pain Assessment and Follow-Up
| 2019 measure. Percentage of visits for patients aged 18 years and older with documentation of a pain assessment using a standardized tool(s) on each visit AND documentation of a follow-up plan when pain is present
|
The Quality Payment Program (for eligible providers and medical groups) currently does not have quality measures related to pressure ulcers/injuries.
* The Percent of Residents or Patients With Pressure Ulcers That Are New or Worsened (Short Stay) (NQF #0678) measure was removed and replaced with the Changes in Skin Integrity Post-Acute Care: Pressure Ulcer/Injury measure, data collection began on July 1, 2018, for Long Term Care Hospitals (LTCHs) and on October 1, 2018, for Inpatient Rehabilitation Facilities (IRFs), for the FY 2020 Quality Reporting Program [4]
** The HACRP is distinct from the Deficit Reduction Act: Hospital-Acquired Conditions (Present on Admission Indicator) program. Hospitals are subject to penalties related to both programs
*** The Quality Payment Program (QPP) was implemented in the U.S. by Medicare in 2017. Merit-based incentive payment system (MIPS) is designed for eligible clinicians who bill under Medicare Part B.
Grayed out measures were deleted/retired
RESOURCES
Official reprint from WoundReference® woundreference.com ©2024 Wound Reference, Inc. All Rights Reserved
NOTE: This is a controlled document. This document is not a substitute for proper training, experience, and exercising of professional judgment. While every effort has been made to ensure the accuracy of the contents, neither the authors nor the Wound Reference, Inc. give any guarantee as to the accuracy of the information contained in them nor accept any liability, with respect to loss, damage, injury or expense arising from any such errors or omissions in the contents of the work.