INTRODUCTION
Background
Definitions
- Patient education is defined as the utilization of an organized process or program by healthcare professionals to provide patients with health information to facilitate learning.[1] Patient education is more than informing or giving information - it includes teaching (Figure 1). Teaching consists of modalities and strategies to facilitate and enhance patients' ability to incorporate what they learn into self-care.[1]
- The goal of patient education is to help individuals improve their health, increase knowledge, and/or influence attitudes.[2] As an outcome, the patient is empowered to manage their condition autonomously to prevent illness, disease, and complications.

Figure 1. Patient education is more than informing or giving information; it includes teaching
Relevance
from a Clinical perspective
- Patients who are fully informed regarding their care and condition(s) are equipped with the knowledge and know-how to be engaged partners in their healthcare.
- Additionally, incorporating patient education into practice:
- Improves patient engagement
- Supports patient-centered care
- Ensures informed decision-making by the patient
- Encourages adherence to prescribed regimens
- Improves health-related outcomes
- Fosters self-care/self-management
- Drives health literacy through improved understanding
from a Quality and safety perspective
- In the U.S., eligible providers are required to participate in the Centers for Medicare and Medicaid (CMS) Quality Payment Program to avoid CMS payment deductions. Among the high priority quality measures that providers can choose from for their performance assessment is the “Consumer Assessment of Healthcare Providers and Systems (CAHPS) for MIPS Clinician/Group Survey”. The Survey, filled out by patients, includes questions related to “Health Promotion & Education”, “Shared Decision Making”, among others. Verbal and written patient education is essential for providers to perform well in this measure.[3]
- Patient education is also a standard for accreditation of healthcare facilities.[4][5] See Table 1.
Table 1. Patient Education Standards for Accreditation by The Joint Commission [6]
Selected Patient Education Standards for Accreditation by The Joint Commission
- Standard PC.02.03.01: The organization provides patient education and training based on each patient's needs and abilities
- EP 1: The organization performs a learning needs assessment for each patient, which includes the patient's cultural and religious beliefs, emotional barriers, desire and motivation to learn, physical or cognitive limitations, and barriers to communication
- EP 5: The organization coordinates the patient education and training provided by all disciplines involved in the patient's care, treatment and services
- EP 10: Based on the patient's condition and assessed needs, the education and training provided to the patient by the organization include any of the following: an explanation of the plan for care, treatment and services; basic health practices and safety; information on the safe and effective use of medications; nutrition interventions and modified diets; discussion of pain, the risk of pain, the importance of effective pain management, the pain assessment process, and methods for pain management; information on oral health; information on the safe and effective use of medical equipment or supplies provided by the hospital; habilitation or rehabilitation techniques to help the patient reach maximum independence; fall reduction strategies
- EP 25: The organization evaluates the patient's understanding of the education and training is provided
- EP 27: The organization provides the patient education on how to communicate concerns about patient safety issues that occur before, during and after care is received
- EP1. The organization assesses the patient’s learning needs.
- EP4. The organization provides education and training to the patient based on the patient’s assessed needs.
- EP5. The organization coordinates the patient education and training provided by all disciplines involved in the patient’s care, treatment, or services.
- EP10. Based on the patient’s condition and assessed needs, the education and training provided to the patient by the organization include the following:
- An explanation of the plan for care, treatment, or services
- Basic health practices and safety
- Information on the safe and effective use of medications
- Nutrition interventions (for example, supplements) and modified diets
- Discussion of pain, the risk for pain, the importance of effective pain management, the pain assessment process, and methods for pain management
- Information on oral health
- Information on the safe and effective use of medical equipment or supplies provided by the organization
- Habilitation or rehabilitation techniques to help the patient reach maximum independence
- EP25. The organization evaluates the patient’s understanding of the education and training it provided.
- EP27. The organization provides the patient education on how to communicate concerns about patient safety issues that occur before, during, and after care is received.
- EP28. For organizations that elect The Joint Commission Primary Care Medical Home option: The primary care clinician and the interdisciplinary team educate the patient on self-management tools and techniques based on the patient’s individual needs.
- EP 30. For organizations that elect The Joint Commission Primary Care Medical Home option: The interdisciplinary team identifies the patient’s health literacy needs.
- EP 31. For organizations that elect The Joint Commission Primary Care Medical Home option: Patient education is consistent with the patient’s health literacy needs.
- Standard RI.01.01.03: The organization respects the patient's right to receive information in a manner he or she understands [6]
- EP 1: The hospital provides information in a manner tailored to the patient’s age, language, and ability to understand
- EP 2: The hospital provides language interpreting and translation services
- EP 3: The hospital provides information to the patient who has vision, speech, hearing, or cognitive impairments in a manner that meets the patient’s needs.
|
What happens if patients are not educated or improperly educated?
- The lack of adequate patient education may result in care and treatment misunderstandings. These misunderstandings may lead to reduced treatment adherence, increased adverse events, medical errors, and the continuation or worsening of symptoms.[7]
- The lack of adherence to medication or treatment regimens is associated with poor clinical outcomes, reduced quality of life, increased hospitalizations, and rising healthcare costs.[7]
PATIENT EDUCATION IN WOUND CARE AND HYPERBARIC OXYGEN THERAPY
What are the current gaps in patient education in wound care and hyperbaric oxygen therapy?
Specific problems in wound care and hyperbaric oxygen therapy (HBOT) patient education include gaps related to limited availability of educational materials, variability in patients’ literacy levels, and complexity of interventions, as described below:
1. There is limited availability of educational materials in wound care and HBOT:
2. Determining Health Literacy and Literacy: Variability in patients’ literacy levels implies that many patients have low literacy skills:
According to the Agency for Healthcare Research and Quality (AHRQ), most Americans struggle to find, understand, and use health information.
[8] A national survey found that 88% of U.S. adults lack the health literacy skills needed to navigate today’s healthcare system, and 36% have limited personal health literacy.[9]
It is important to differentiate health literacy from language proficiency.
[10] Individuals with limited language proficiency experience similar problems to those with limited health literacy, such as delay or denial of services, issues with medication management, and underutilization of preventive services.[11]
- Literacy: low literacy skills may inhibit understanding of the patient's own condition and care plan.
- Literacy includes the ability to read and write, as well as comprehend, problem solve, and reason.[1] Patient education visual aids ideally should be created at a fifth-grade reading level or less and include simple pictorials and limited words.[12]
- Health literacy: low health literacy skills may impede adherence to the wound care plan and consequently delay wound closure.
- Personal health literacy is defined as the capacity to process, understand, and obtain health information and services to inform health-related decisions and actions for themselves and others.[13][14] Patients with low to moderate health literacy skills struggle with self-management.[15]
- In other conditions with similar multi-step self-care regimens (e.g. diabetes, heart failure), lower health literacy is associated with reduced disease knowledge, self-efficacy, and self-care behaviors.[16][17]
- Within wound care, health literacy research is limited.[15] A prospective cohort study reported that patients with lower health literacy had larger and older wounds compared to those with higher health literacy.[18]
- To determine health literacy of patient and patient's families/caregivers (e.g., reading comprehension and level, language, cognition), several validated tools have been developed. Examples of these tools include:
- Newest Vital Sign (NVS): A brief health literacy screening tool in which patients answer six questions based on a nutrition label from an ice cream container. The questions assess reading comprehension and numeracy skills, including the ability to interpret basic text and perform simple mathematical calculations. The NVS is available in multiple languages.[19]
- Rapid Estimate of Adult Literacy in Medicine (REALM): A health literacy screening tool that measures a patient’s ability to recognize and pronounce common health-related terms. It provides an estimated reading grade level (up to ninth grade) based on word recognition. [20]
- Brief Health Literacy Screening Tool (BRIEF): A brief, subjective health literacy screening tool consisting of three self-report items that assess a respondent’s confidence in completing medical forms independently, difficulty learning about medical conditions due to written information, and need for assistance understanding health-related materials. [21]
- The utility of health literacy screening tools is debated. Some argue against individually assessing patients' skills with these tools, citing widespread limited health literacy based on national data.[22] Others believe the tools remain valuable in clinical practice.[23]
- Regardless of this debate, and despite the scarcity of patient information written at the fifth or sixth-grade level [22], clinicians and health systems should prioritize providing all patients with universally easy-to-understand information, irrespective of their reading level or background.[22][10]
- The AHRQ provides comprehensive resources for Health Literacy Professional Education and Training, including the AHRQ Health Literacy Universal Precautions Toolkit.
- Key health literacy best practices include [14]:
- Use of plain language to enhance reading comprehension
- Use of your audience's preferred language and communication channels
- Use of culturally and linguistically appropriate language
- Organizational health literacy is the degree to which organizations equitably enable individuals to find, understand, and use information and services to inform health-related decisions and actions for themselves and others. Examples include organizations using the Teach-Back method to ensure patient comprehension.[13][14]
- Digital health literacy is the ability to seek, find, understand, and appraise health information from electronic sources and apply the knowledge gained to addressing or solving a health problem. Examples include patients communicating electronically with the health care team.[13][14]
- For details, refer to section 'Linguistic Access and Health Literacy' in topic "Culturally and Linguistically Appropriate Services in Wound Care".
3. Complexity of many wound care/ HBOT interventions require that patients who perform self-care at home be knowledgeable and skilled:
- Advancements in wound care technology coupled with improved dressing application methods have led to multi-step dressing regimens individualized to a patient’s specific wound characteristics. As a result, dressing change regimens require multiple steps, are scheduled at specific intervals, and require knowledge and skill in removal and application.
- Increasingly, patients (and family members and caregivers) are responsible for performing these complex regimens themselves in the home. If not performed correctly, patients are at risk for adverse outcomes such as infection, delayed healing, and increased dressing costs.
- Healthcare professionals must teach these complex regimens in an effective manner that supports the development of dressing skills, knowledge of complications (ex. infection monitoring), and adherence to the dressing change regimen.
What are the most commonly used methods for patient education?
Typical patient and family education strategies include print, audio-visual methods, demonstration, and verbal instruction.
[5] Among these strategies, verbal education is used in virtually every patient-provider encounter. When effective, verbal patient education has been shown to improve the patient’s ability to care for him or herself after discharge, thus reducing morbidity and mortality.[5] However, not all patients learn effectively through verbal instructions. Different people learn differently, and providers need to adapt their teaching style to the patient’s needs.[5]
- For all patients/ caregivers, especially patients whose preferred learning style is not verbal communication, pictures on paper or on a screen may serve as simple visual aids to supplement verbal education.[5][24]
- Systematic reviews have shown that:
- Caregivers/ patients who receive written and verbal information are more knowledgeable and satisfied than those that receive verbal education alone.[25]
- Written information provided as new patient information packages or booklets improved patient knowledge and reduced confusion.[26]
- The use of customized print material resulted in better information recall than did general print materials, and evidence-based brochures increased knowledge compared to no brochures.[27]
The Teach Back Method
The teach-back method is an evidence-based approach to health literacy that is integral to promoting patient safety, quality of care, adherence, and engagement.[28][29] This method is considered a universal health-literacy precaution and should be used with every patient, regardless of education level or experience with wound care.[30]
This technique involves asking the patient or their family caregiver to explain, in their own words, the information they received or the actions they need to perform. Essentially, teach-back serves as a confirmation method: it verifies that the health information was communicated clearly and that the patient or caregiver has achieved a clear understanding of the instructions given.[28]
- Use open-ended questions rather than “yes” or “no” questions.[29] Examples:
- “I want to be sure I explained everything clearly. Can you show me how you’ll change this dressing at home?”
- “Tell me in your own words what you would do if this wound becomes red, swollen, or has more drainage.”
- Avoid yes/no questions like “Do you understand?”[29]
The Educate Model
The Brigham and Women’s Faulkner Hospital in Boston developed a model to facilitate verbal patient and family education. The EDUCATE model provides best practices for clinicians who need to educate patients and caregivers.
[5] Figure 1 provides a framework based on the EDUCATE model, that wound care and HBOT clinicians can use to enhance verbal education in any care setting.
How can patient education in wound care help improve outcomes?
Patient education has a direct relationship to adherence: research cites improved patient adherence as an outcome when effective education is given.[1][7]
Adherence to care plans has many forms and is important in all healthcare settings. Issues in adherence may appear in the form of non-adherence or limited adherence to medication, treatments, appointment keeping, dietary, and lifestyle measures.
[1] Adherence is influenced by factors that are related to the healthcare system or the patient.- Healthcare factors that influence adherence include the lack of adequate or effective patient teaching, poor communication, a non-patient-centered approach, and a lack of consideration of the influence of the socio-cultural aspects of the patient.[1]
- Patient-based factors associated with adherence include literacy, health literacy, psychosocial, environmental, developmental, cultural, and communication factors.[1]
Literature shows that educational interventions in wound self-care improve outcomes. Below we summarize studies that support the integration of patient education interventions to foster wound self-care. In general, findings of these studies suggest that patient education results in increased adherence to wound care plans and better outcomes:
- A prospective study incorporating a home-based venous ulcer patient education program reported reduced venous ulcer recurrence rates and improved disease knowledge and self-care.[31]
- In the emergency room setting, a 25-minute education program focused on wound self-care management of lacerations with practice on a prosthetic model and a booklet resulted in increased satisfaction in wound care, improved self-care, and reduced infection rates.[32]
- Similarly, a wound education pilot that utilized individualized literacy-supportive visual aids and prosthetic models found a significant improvement in knowledge, dressing performance, and healing in English and Spanish-speaking patients with variable health literacy levels.[33]
- In a randomized control trial by Chan and Lai [34], a patient education program that incorporated patient teaching and telephone follow-up for wound care in the home-setting by patients compared to dressing changes by professional nurses in an outpatient clinic showed no differences in wound healing.
Effective patient education improves adherence.
How can patient education in wound care help improve patient satisfaction survey scores?
Below are examples of patient satisfaction surveys that have been used in wound care.[35][36][37] Patient education is a main component of resulting scores.
Press Ganey
Asks patients to rate their experience with a doctor, physician assistant (PA), nurse practitioner (NP) or specialist in areas such as [35]:
- Friendliness/courtesy
- Explanations the care provider gave the patient about the problem or condition
- Concern the care provider showed for the patient's questions or worries
- Ability to include the patient in decisions about his/her care
- Explanation on the treatment and follow up instructions
- Ability of the care provider to use words the patient can understand
- Amount of time spent with the patient
- Confidence placed in the care provider
- Likelihood of recommending the provider to someone else
- Cared about you?
- Included you in decisions about your care?
- Showed concern about your problem or condition?
- Clearly explained your problem or condition?
- Clearly explained your treatment and follow-up instructions?
- Addressed your questions and concerns?
Client Satisfaction Questionnaire (CSQ-8)
Presents questions such as [36][37]:
- Were you happy with the quality of service?
- Were you happy with the kind of service?
- To what extent has the service met your needs?
- Would you recommend the service to a friend?
- Were you happy with the amount of help received?
- Were your problems dealt with?
- Overall, were you satisfied with the service?
- Would you come back?
What factors should be considered when developing patient educational programs in wound care and/or HBOT?
When developing an educational program, factors to be considered include the needs of the target patient population, education content, and logistics of how/ when/ who will deliver the education intervention.
- Teaching interventions that promote adherence includes: 1) assessment of the learning needs of each patient, 2) incorporation of best practices for information presentation, and 3) adjustment of the education to support patient-specific needs and circumstances.[1] (See Figure 2 above for details)
- Teaching interventions should be patient-centered and address patient-related adherence issues that hinder proper self-care. A patient-centered approach encourages healthcare professionals to engage in shared-decision making.
WoundReference clinical and reimbursement decision support web-app offers a comprehensive set of tools and content to enhance verbal patient education and promote patient adherence. For a list of tools and content (Free and Premium), proceed to the section below.
CLINICAL DECISION SUPPORT AND PATIENT EDUCATION
WoundReference clinical and reimbursement decision support platform offers a comprehensive suite of features to facilitate patient education at the point-of-care and at the patient’s home. WoundReference’s solutions allow clinicians to enhance verbal education with written and visual aids, in order to improve patient knowledge, satisfaction, adherence and wound healing outcomes.
[33][25] WoundReference's Patient Education Features: 5 tools to enhance patient engagement
1. Dressing Change Brochure Editor
(Free Basic Plan and above)
The Dressing Change Brochure Editor in
English and in
Spanish is a digital tool was based on a paper-based visual aid that was previously piloted and optimized for English and Spanish-speaking populations, at a 5th grade level (Figure 3).
[38][33] Figure 3. Custom patient handout instantly created with the Dressing Change Brochure Editor
With this digital, point-of-care dressing education tool clinicians can:
- Edit brochures on-the-fly and set their patients up for successful dressing changes at home. Select from ~50 different professional pictures to compose brochures specific to each patient.
- Empower patients to engage in self-care through customized, pictorial, step-by-step instructions
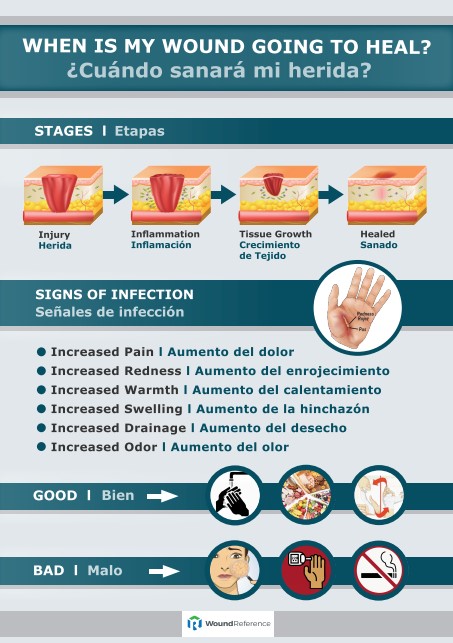
Figure 4. Wound Poster "When is My Wound Going to Heal?"
3. Instant Personalized Product Handouts
(Premium)
To adhere to care plans, patients need to know which products to purchase, where to obtain them, how much they cost, and how to use them.
[39] The Instant Personalized Product Handouts Generator is a point-of-care digital tool allows clinicians to instantly generate product handouts with clinical, coverage, supplier information customized to patients (Figure 5).
Figure 5. Sample product handout. Brand names have been blurred. WoundReference does not advertise or commercialize products used on patients
4. Custom Patient Education Handouts with the Wound Care and/or HBOT Program’s Logo
(Premium)
This point-of-care, digital education tool automatically adds the Program’s logo to WoundReference’s evidence-based wound care brochures. Examples include "
Venous Leg Ulcer" and "
Diabetic Foot Ulcer"
- Evidence-based brochures improve patient knowledge, reduce confusion and increase satisfaction.[26][27][25]
- Branded brochures backed by evidence and updated as needed reinforces the Program’s authority and reputation among patients, caregivers, and healthcare professionals.
5. Patient Education Handouts for Patients Undergoing HBOT in English and Spanish
(Premium)
The WoundReference Editorial Team has been creating patient education handouts for the most common HBOT indications. The growing library contains illustration-rich handouts in English and Spanish written at a 5th grade level, to facilitate comprehension by patients and caregivers. Handouts can be printed with a regular printer at the point-of-care or digitally shared with patients and caregivers. For a list of available handouts, see "
HBO Education Materials for Patients".
OTHER RESOURCES
Official reprint from WoundReference® woundreference.com ©2026 Wound Reference, Inc. All Rights Reserved
NOTE: This is a controlled document. This document is not a substitute for proper training, experience, and exercising of professional judgment. While every effort has been made to ensure the accuracy of the contents, neither the authors nor the Wound Reference, Inc. give any guarantee as to the accuracy of the information contained in them nor accept any liability, with respect to loss, damage, injury or expense arising from any such errors or omissions in the contents of the work.