Use of compression therapy to reduce edema in patients with complex chronic leg ulcers is often challenging, and in some situations, contraindicated. Circumferential Negative Pressure Wound Therapy (NPWT) has been successfully used for edema control in lower extremity fractures [1][2] and to bolster skin grafts in male genital reconstruction.[3] It may also be a viable alternative for patients with chronic leg ulcers and coexistent edema who have failed to respond to standard compression treatment, and for whom traditional compression devices (i.e, bandages, wraps) are not an option due to factors such as patient inability to tolerate therapy, refusal, or difficult limb dimensions.
The 2 cases below illustrate the first author's experience with use of circumferential NPWT for management of complex ulcers: Case 1 describes use of circumferential NPWT to treat lower extremity ulcers in a patient with lipedema and lipodermatosclerosis, and includes pictures of the technique. Case 2 describes how circumferential NPWT was used to treat a non-healing ulcer on a lower extremity stump.
CASES
Case 1: Lipedema and lipodermatosclerosis
Case presentation:
History of Present Illness
A 62 year old female patient was referred to the wound clinic of a community hospital due to multiple recalcitrant ulcerations in both legs, accompanied by severe pain, mild edema and mild erythema that started 14 months prior to her referral to the wound clinic. The patient had been treated by her primary care physician and a dermatologist for cellulitis, lipodermatosclerosis and stasis dermatitis, however her pain only worsened and ulcers had not shown any signs of improvement.
Pertinent Medical History
The patient had rheumatoid arthritis (RA) and a foot deformity that had been surgically treated by Podiatry 2 years prior. Postoperatively, she developed a deep venous thrombosis (DVT) in her right lower extremity, phlebitis in her left lower extremity and was subsequntly treated with warfarin. An ultrasound performed 6 months later showed resolution of DVT. Additionally, the patient had interstitial lung disease, and was taking azathioprine, prednisone, aspirin and furosemide. She had no history of smoking.
Physical Exam
Upon local wound exam, patient presented with painful, full-thickness ulcers in both legs, covered with necrotic tissue (Figures 1-4).
Diagnostics
Her lab values were suggestive of anemia, inflammatory process, decreased renal function, and abnormal liver function. She had a prior vein mapping showing right sided peripheral venous insufficiency. Her wound cultures were positive for Klebsiella and Proteus Vulgaris, but fungal and acid-fast bacili (AFB) cultures were negative.
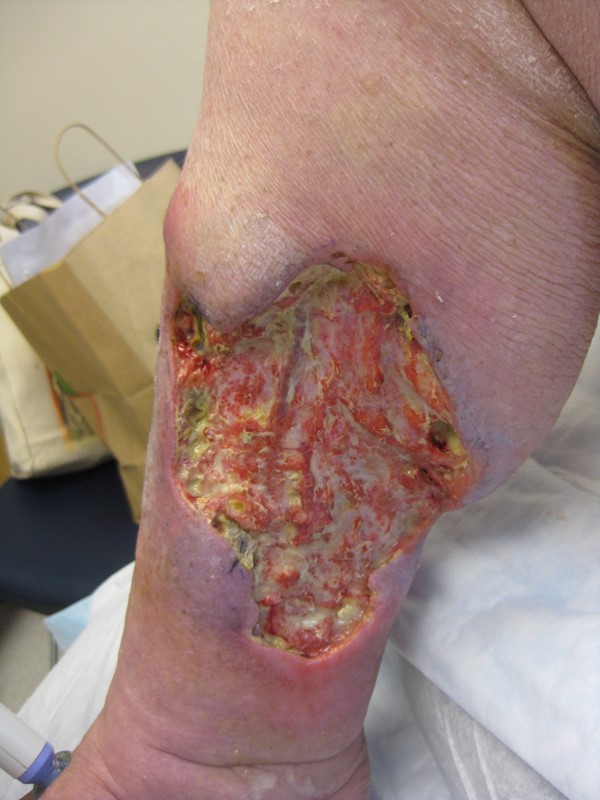
Figure 1. Right medial lower leg | 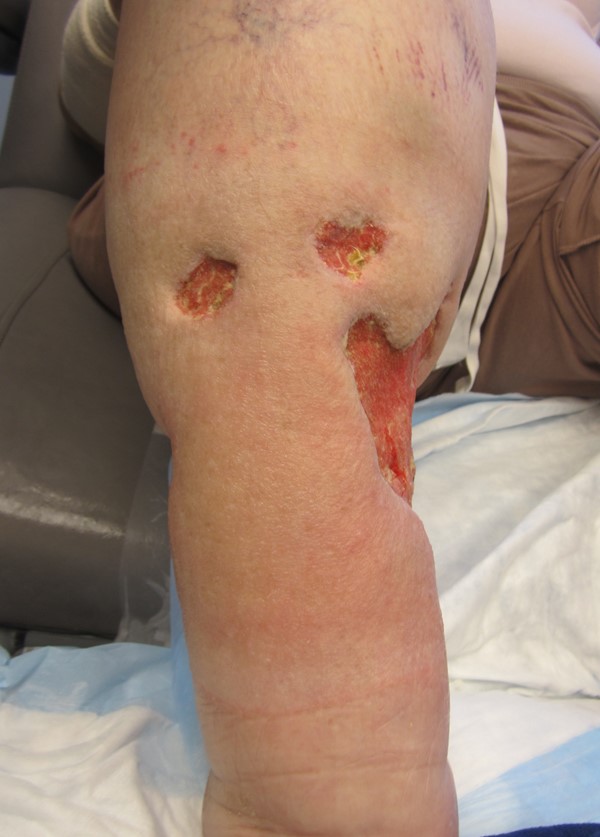
Figure 2. Right lower leg |
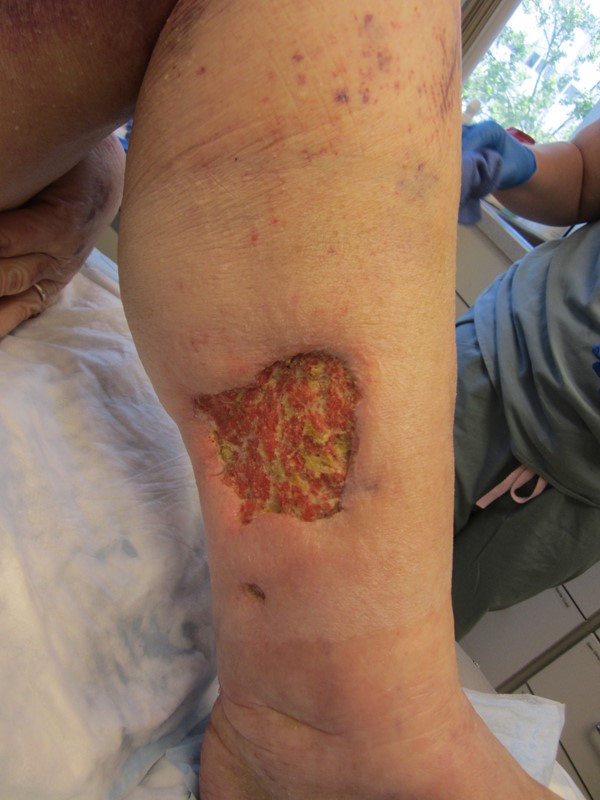
Figure 3. Left medial lower leg | 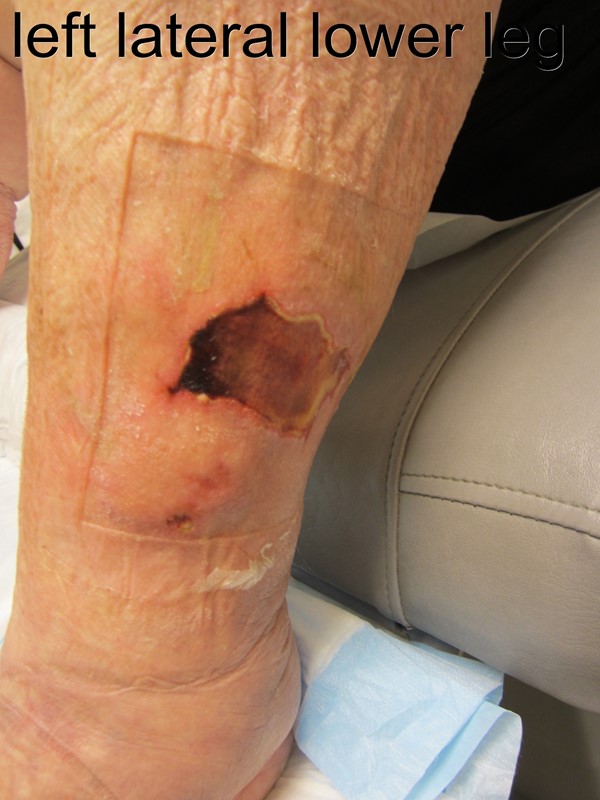
Figure 4. Left lateral lower leg |
Wound Management and Patient Outcome:
Initial compression therapy with bandages was attempted, however patient did not tolerate any level of compression due to severe pain and and propensity to develop new ulcerations. Surgical debridement was performed and soon after, circumferential NPWT was initiated. At each dressing change, ulcers were cleansed and moisturizer was generously applied on the periwound skin. Saline-moist antimicrobial gauze circumferential dressing and NPWT was applied at 90 mmHg, at continuous setting. Ideally, both legs would have been dressed from toes to right below knee, however the patient did not tolerate any dressings on her feet due to severe pain. Dressings were changed twice a week in the clinic for the first 3 weeks, then by home health with a follow up appointment in the clinic. No analgesics were required during dressing changes, as gauze was still moist and could be easily removed. Within a week, a marked reduction in both edema and pain was observed. At the 3rd week, ulcers assessment revealed a clean granular wound bed, and partial closure of ulcers was seen within 8 weeks. Ulcers were completely closed by 6 months since initiation of treatment at the wound clinic.
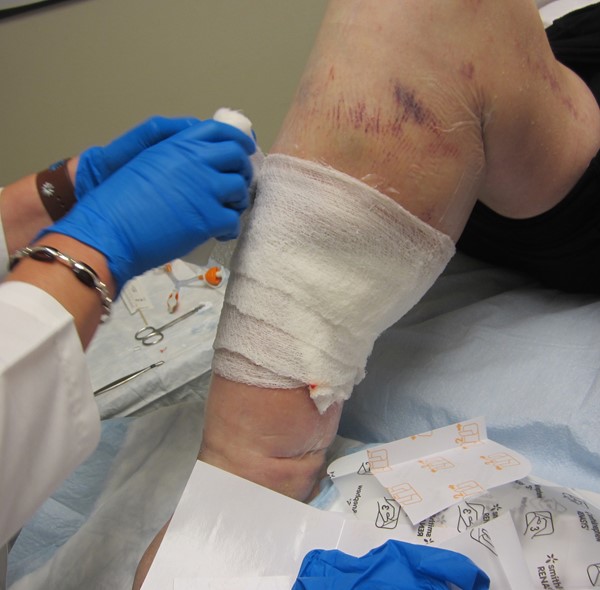
Figure 5. Saline-moist antimicrobial gauze on periwound film | 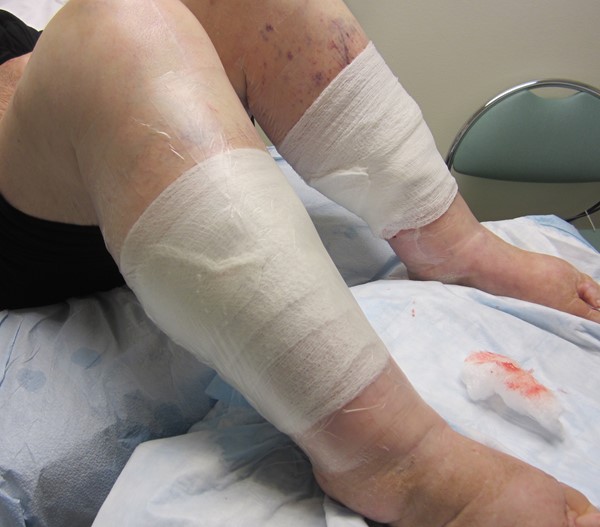
Figure 6. Film applied over moist gauze |
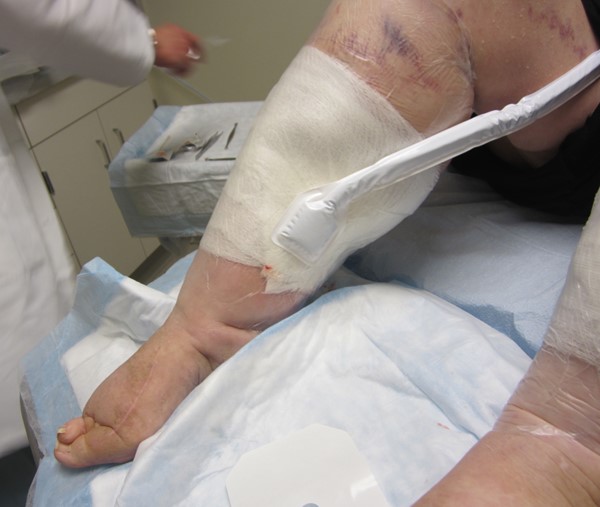
Figure 7. NPWT tubing applied | 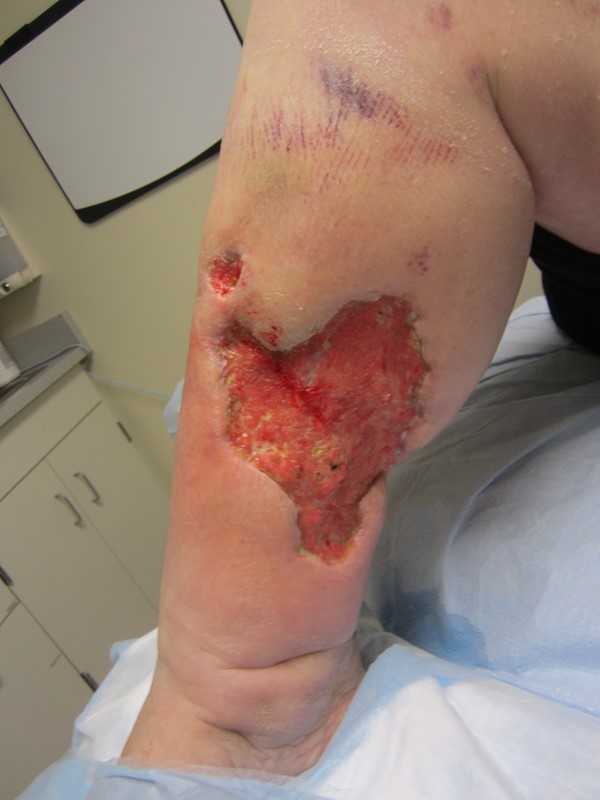
Figure 8. Wound contraction and granulation, week 3 |
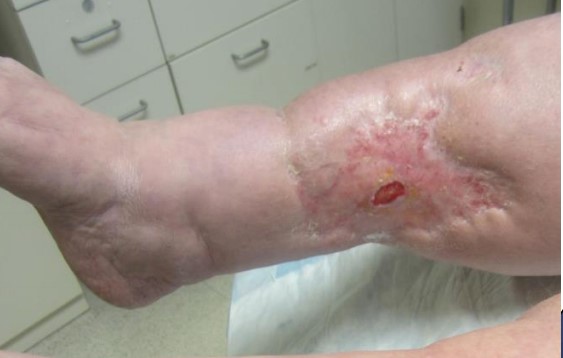
Figure 9. Right medial leg ulcer almost healed, week 8 |
|
Case 2: Ulcer on lower extremity stump
Case presentation:
History of Present Illness
56 year old male patient presented to the wound clinic with a history of non-healing ulcer in his right lower extremity stump. The patient underwent below the knee amputation and coverage with posterior myocutaneous flap 2 months prior to his first visit to the wound clinic. The upper incision line dehisced due to excessive tension 2 weeks after his surgery and the wound was treated conservatively for 4 weeks with no signs of improvement.
Pertinent Medical History
The patient had diabetes and peripheral artery disease.
Physical Exam
Upon local wound exam, patient presented with one full-thickness ulcer in the cranial, frontal aspect of the incision line, measuring approximately 5cm (width) x 2 cm (length) x 2 cm (depth). Wound had granulation tissue and moderate quantity of serosanguinous exudate (Figure 10).
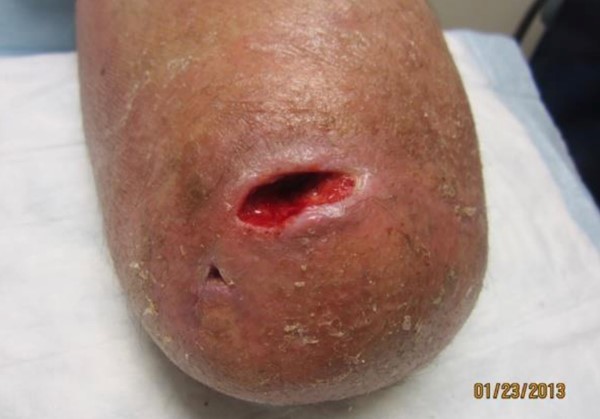
Figure 10. Non-healing ulcer on stump
Wound Management and Patient Outcome:
Circumferential NPWT was applied using the same technique described for Case 1. Dressing changes were performed 2 times per week in the clinic for 2 weeks, then managed by home health. Ulcer healed completely after 6 weeks and patient was able to wear his prosthesis. This technique also helped shrink the stump.
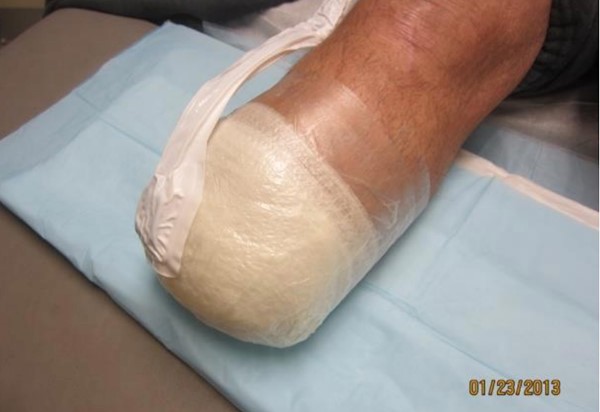
Figure 11. Circumferential NPWT on stump
DISCUSSION
Use of circumferential NPWT has been reported in literature as an effective alternative to manage pre and postoperative edema in lower limb fractures.[1][2] It has also been reported as a method to bolster skin grafts in male genital reconstruction (Figure 12) - in those cases, circumferential NPWT applied to the penis facilitated skin grafting to the complex contour of male genitalia, without decrease in perfusion or avascular necrosis.[3]
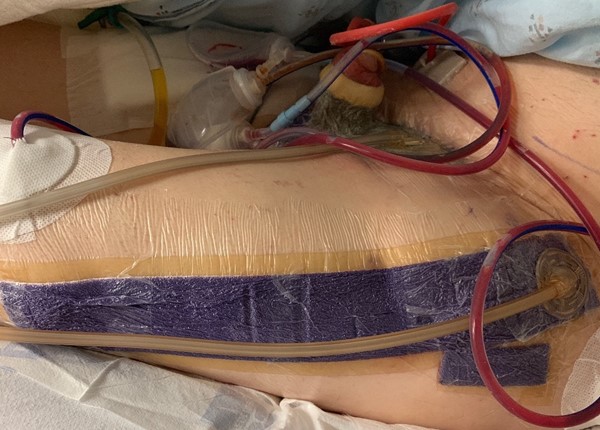
Figure 12. Circumferential NPWT to bolster skin graft in male genital reconstruction (top, center). A flap (tensor fascia lata) was used for scrotal reconstruction. By Kuplicki S, MSN, APRN.
Here we presented two other cases that benefited from circumferential NPWT. Case 1 (lipedema) represents a complex case of chronic ulcer with multiple co-morbidities and medications that impair wound healing, in addition to patient intolerance to standard therapies (i.e, compression bandages to reduce edema). As ulcers were refractory to standard treatment and no other options were available, circumferential NPWT appeared as an attractive alternative for this case. Case 2 (stump) is an example of an ulcer that is difficult to dress/heal, in a patient with multiple co-morbidities.
NPWT may effectively assist with edema management by removing interstitial fluid, which fills the spaces between most cells and comprises a substantial portion of the fluid environment in the body. However, common concerns include disruption of soft tissue integrity or decrease in blood perfusion distally to the area treated with circumferential NPWT.[4] Barandse-Hofmann et al [1] have found that circumferential NPWT did not disrupt healthy soft tissue integrity when treating a patient with a large degloving limb ulcer. The first author has not encountered this side effect in none of the cases treated with circumferential NPWT so far either. In fact, one of the reasons why the author chose to use circumferential NPWT in Case 1 (lipedema) was to maintain soft tissue integrity, which had been disrupted by traditional compression therapy (i.e. new ulcer formation).
As for the potential to decrease distal blood supply, it is suggested that NPWT should be used with caution on tissues with compromised vascularity, particularly when used circumferentially.[4] Manufacturers recommend use of circumferential NPWT dressings only in the presence of anasarca or excessively weeping extremities, where a circumferential film technique may be necessary to establish and maintain a seal. We agree that circumferential NPWT should be applied with caution, and distal circulatory status should be frequently and systematically monitored.[5] If decreased pulses or perfusion are suspected, circumferential NPWT should be immediately discontinued. Other techniques that minimize risk include use of multiple small pieces of transparent film rather than one continuous piece, loosely attaching the edges without stretching or pulling the film when securing it. [5]
In summary, in her experience the author has found that circumferential NPWT leads to substantially improved wound healing and markedly decreased pain in complex cases like the ones described herein. Circumferential NPWT may be an alternative for complex chronic leg ulcers that are refractory to standard treatment and for which traditional compression therapy is not an option.