Last updated on 3/30/26 | First published on 7/27/18 | Literature review current through Apr. 2026
[cite]
Authors:
Elaine Horibe Song MD, PhD, MBA,
Kathryn Whiston-Lemm ACNP, CWON-AP,
Julie Lientz MSN, MBA, RN, WCC, CWON,
Kim Simonson RN-BC, ACHRN, CWS, FACCWS,
more...
Coauthor(s)
Elaine Horibe Song, MD, PhD, MBACo-Founder and Editor, Wound Reference, Inc;
Professor (Affiliate), Division of Plastic Surgery, Federal University of Sao Paulo;
Volunteer, Association for the Advancement of Wound Care;
Google Scholar Profile
Disclosures: Nothing to disclose
Kathryn Whiston-Lemm, ACNP, CWON-AP
Disclosures: Nothing to disclose
Julie Lientz, MSN, MBA, RN, WCC, CWON
Disclosures: Nothing to disclose
Kim Simonson, RN-BC, ACHRN, CWS, FACCWS
Disclosures: Nothing to disclose
Editors
INTRODUCTION
Background
Venous leg ulcer (VLU) can be defined as an open skin lesion of the leg or foot that occurs in an area affected by venous hypertension.[1] (See Figure 1)
Guidelines, Quality Measures and resources for VLU prevention, assessment and management are listed below. For and introduction and assessment of venous leg ulcers (VLU) including epidemiology, risk factors, etiology, pathophysiology, history, physical examination, diagnosis, differential diagnoses, documentation and ICD-10 coding, see "Venous Ulcers - Introduction and Assessment". For VLU management including a section for clinicians on patient education, see "Venous ulcers - Treatment and Prevention". For an overview of surgical interventions that can be performed in outpatient settings (e.g. office-based settings and vein clinics) for management of chronic venous disease and resulting manifestations such as VLUs, see " Chronic Venous Disease - Surgical Management".
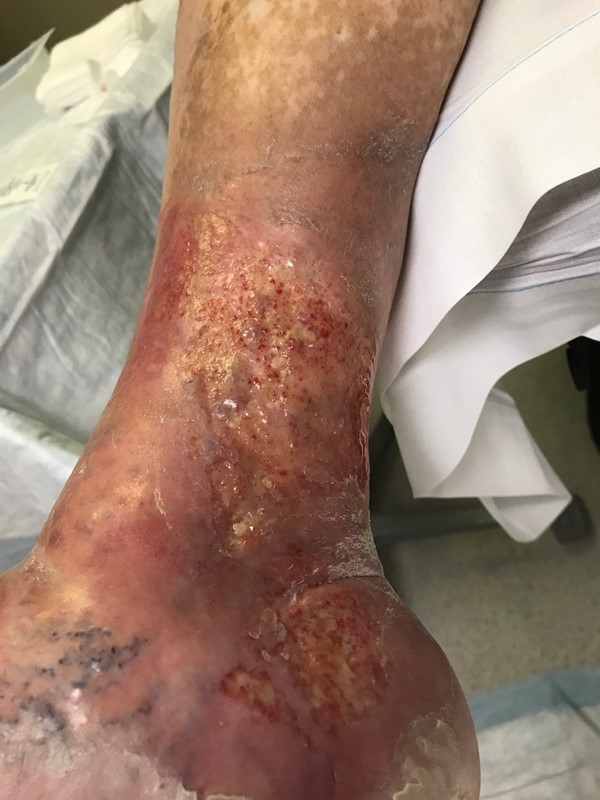
Figure 1. Highly exudative venous ulcer
Relevance
- Approximately 1% of the population in the United States, 3% of people over 80 years of age in westernized countries.[2] Prevalence is increasing, coinciding with an aging population. In the U.S., VLUs affect between 500,000 to 2 million people per year [3].
- VLUs can result in pain, unpleasant odor, reduced mobility, sleep disturbance, reduced psychological well-being and social isolation.[4] In severe cases and when associated with arterial insufficiency, VLUs can lead to limb amputation. [5][6]
- Despite the relatively low prevalence, VLUs represent a significant financial burden to the healthcare system in the U.S., estimated to be between US$ 2 and 2.5 billion per year. [1][7] One study estimated the overall burden to Medicare and private insurers due to VLU in the U.S. (excluding out-of-pocket payments and other indirect costs such as lost productivity) to be of US$14.9 billion (in 2012 US$ ). [8] In the U.K., estimated costs to treat a person with open leg ulcer is around GBP 1700 (US$ 2122) per year at 2012 prices, mostly related to nursing time. [9]
EVIDENCE-BASED CLINICAL GUIDELINES
Below is a list of the some of the most recent evidence-based guidelines on VLU:
| Evidence-based guideline, Year |
Publishing Organization, Country or Region |
Links |
| Clinical Guidelines on Compression Therapy in Venous Diseases, 2025 | Annuals of Vascular Surgery | Guideline (paid) |
| Wound, Pressure Ulcer, and Burn Guidelines-5: Guidelines for the management of lower leg ulcers and varicose veins, second edition, 2024 | Japanese Dermatological Association, Japan | Guideline (free) |
Diagnosis and treatment of venous leg ulcers: S2k Guideline of the German Society of Phlebology and Lymphology (DGPL) e.V., 2024 [10]
| German Society of Phlebology and Lymphology (DGPL)
| Guideline (free) |
| ACR Appropriateness Criteria® Lower Extremity Chronic Venous Disease, 2023 | American College of Radiology | Guideline (free) |
The 2023 Society for Vascular Surgery, American Venous Forum, and American Vein and Lymphatic Society clinical practice guidelines for the management of varicose veins of the lower extremities. Part II, 2023 [11]
| Society for Vascular Surgery, American Venous Forum, and American Vein and Lymphatic Society
| Guideline (free) |
The 2022 Society for Vascular Surgery, American Venous Forum, and American Vein and Lymphatic Society clinical practice guidelines for the management of varicose veins of the lower extremities. Part I. Duplex Scanning and Treatment of Superficial Truncal Reflux: Endorsed by the Society for Vascular Medicine and the International Union of Phlebology, 2022 [12]
| Society for Vascular Surgery, American Venous Forum, and American Vein and Lymphatic Society
| Guideline (free)
|
Editor's Choice – European Society for Vascular Surgery (ESVS) 2022 Clinical Practice Guidelines on the Management of Chronic Venous Disease of the Lower Limbs, 2022 [13]
| European Society for Vascular Surgery (ESVS)
| Guideline (free) |
2019 Guideline for Management of Wounds in Patients With Lower-Extremity Venous Disease (LEVD) [14]
| Wound, Ostomy and Continence Nurses Society | Guideline (paid) |
Compression therapy after invasive treatment of superficial veins of the lower extremities: Clinical practice guidelines of the American Venous Forum, Society for Vascular Surgery, American College of Phlebology, Society for Vascular Medicine, and International Union of Phlebology, 2019 [15]
| American Venous Forum, Society for Vascular Surgery, American College of Phlebology, Society for Vascular Medicine, and International Union of Phlebology
| Guideline (free)
|
Evidence-based (S3) guidelines for diagnostics and treatment of venous leg ulcers, 2016 [16]
| European Dermatology Forum, Europe
| Guideline (free)
|
Wound healing society 2015 update on guidelines for venous ulcers, 2015 [17]
| Wound Healing Society, USA
| Guideline (free)
|
The International Consolidated Venous Ulcer Guideline Update, 2015 [18]
| Association for the Advancement of Wound Care (AAWC), Wound Healing Society, and the Canadian Association for Enterostomal Therapy formed the International Consolidated Guidelines Taskforce, North America
| Guideline (free)
|
Management of venous leg ulcers: Clinical practice guidelines of the Society for Vascular Surgery (SVS) and the American Venous Forum (AVF), 2014 [1]
| The Society for Vascular Surgery and American Venous Forum, USA
| Guideline (free) |
QUALITY MEASURES
Relevant Quality Measures are listed below. For CMS MIPS measures, benchmarks are available on the CMS Quality Payment Program Measures Benchmarks.
| Setting |
CMS Program |
Developed by |
Measure ID |
Title |
Description/ benchmark (when available) |
Outpatient
| Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| US Wound Registry
| USWR22
| Nutritional Assessment and Intervention Plan in Patients with Wounds and Ulcers | The percentage of patients aged 18 years and older with a diagnosis of a wound or ulcer of any type who self-report nutritional screening with a validated tool (such as the Self-MNA® by Nestlé) as well as food insecurity assessment, AND for whom the clinician provides and documents a follow up/ intervention plan within the 12-month reporting period.
|
Outpatient
| Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| US Wound Registry
| USWR30
| Non Invasive Arterial Assessment of patients with lower extremity wounds or ulcers for determination of healing potential
| Percentage of patients aged 18 years or older with a non healing lower extremity wounds or ulcers that underwent a non-invasive arterial assessment once in a 12 month period, stratified by ABI, perfusion pressure, or oximetry. Data from the USWR indicates that fewer than 10% of patients with chronic non-healing leg ulcers undergo any type of vascular assessment (ABI, transcutaneous oximetry or skin perfusion pressure) even at hospital based outpatient wound centers. In 2020, clinician performance ranged from 0% to 100% with an average of 57.6% for practitioners that submitted data to CMS 44.6% among clinicians who did not submit quality data, suggesting that QCDR participation improves the performance of arterial screening.
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (*) | US Wound Registry | USWR32 | Adequate Compression of Venous Leg Ulcers (VLU) at each treatment visit, appropriate to arterial supply | Percentage of venous leg ulcer visits among patients aged 18 years and older in which adequate compression is performed at each treatment visit in the 12 month reporting period or until VLU outcome . Arterial status must first be assessed at least one time with any non-invasive method and the device chosen for compression must be appropriate based on whether arterial supply is normal or reduced (see: USWR30: Arterial Screening Measure). As a benchmark, among providers reporting this measure, performance is more than 70% of visits. However, among providers who do NOT report the measure, compression is provided in only 25% of VLU visits. |
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (*) | US Wound Registry | USWR34 | Venous Leg Ulcer (VLU) Healing or Closure | Percentage of venous leg ulcers among patients age 18 or older that have achieved healing or closure within 12 months, stratified by the Wound Healing Index (WHI).Healing or closure is defined as complete epithelialization without drainage or the need for a dressing over the closed ulceration, although venous compression would still be required. As a benchmark, performance rate in 2016 was 19% for WHI 1, 35% for WHI 2, and 54% for WHI 3. In 2018, the average performance rate for clinicians reporting this measure to CMS was 64%. In 2020, the average performance rate was only 23%. It seems likely that the low average performance rate in 2020 was due to low participation but COVID had a profound impact on patient visit frequency, patient volume, etc. at outpatient wound centers. The USWR actually has over 100 practitioners who report this measure internally if not to CMS, and the numbers for the entire group regardless of MIPS reporting are: 2018: Ave rate 61%; 2019: ave. performance 40%; 2020; Ave. 42%. |
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (*) | US Wound Registry | USWR37 | Objective Measurement of Wound Surface Area with AI-based Imaging | Percentage of chronic wound/ulcer treatment visits in which wound surface area is measured objectively with an AI-based imaging tool, allowing for an objective evaluation of surface area reduction over time. |
Outpatient
| Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| Medicare
| MIPS 128 (not for traditional MIPS)
| Preventative Care and Screening: Body Mass Index (BMI) Screening and Follow-Up
| Percentage of patients aged 18 years and older with a BMI documented during the current encounter or during the previous twelve months AND with a BMI outside of normal parameters, a follow-up plan is documented during the encounter or during the previous twelve months of the current encounter
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| National Committee for Quality Assurance
| MIPS 155
| Falls: Plan of Care
| Percentage of patients aged 65 years and older with a history of falls that had a plan of care for falls documented within 12 months.
|
| Retired |
|
|
|
|
|
| Setting | CMS Program | Developed by | Measure ID | Title | Description/ benchmark (when available) |
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (*) | US Wound Registry | CDR3 | Process measure: Plan of Care Creation for Diabetic Foot Ulcer (DFU) and Venous Leg Ulcer (VLU) not Achieving 30% Closure at 4 Weeks
| 2019 measure. A plan of care needs to be created for patients that fail to achieve 30% of wound closure within 4 weeks of the application of the first CTP, and will include review of whether appropriate usual care has been implemented as well as whether further CTP applications are indicated
|
| Outpatient | Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| US Wound Registry
| CDR9 | Appropriate use of Cellular and/or Tissue Based Product (CTP) in diabetic foot ulcers (DFUs) or venous leg ulcer (VLUs) among patients 18 years or older
| 2019 measure. Percent of patients 18 or older with venous or diabetic foot ulcer who receive cellular and/or tissue based products (CTPs) appropriately. Appropriate Use of CTPs for a DFU or VLU is defined as use that adheres to Medicare coverage policy regarding the total number of applications over a specific timeframe. Regional Medicare Administrative Carrier (MAC) policies differ but using the most restrictive Local Coverage Determination (LCD), appropriate use is defined as: No more than 10 applications per wound, CTP applications do not continue if the wound is unchanged in size or larger in size after 4 weeks have elapsed from the first application, CTP applications do not continue once the wound is 0.5 cm2 or smaller. Prior to application of a CTP, patient should undergo vascular assessment to exclude ischemia, control bioburden, and debride necrotic material, as well as provide other appropriate basic interventions such as compression of a venous ulcer or offloading of a diabetic foot ulcer. Currently the benchmark rate is only 23%.
|
Outpatient
| Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| US Wound Registry
| USWR24
| Patient Reported Experience of Care: Wound Outcome
| All eligible patients with wounds or ulcers who completed of Wound Outcome Questionnaire who showed 10% improvement at discharge or transfer to another site of care during the 12 month reporting period.
|
Outpatient
| Quality Payment Program - Merit-based incentive payment system (MIPS) (*)
| Medicare | MIPS 131
| Pain Assessment and Follow-Up
| 2019 measure. Percentage of visits for patients aged 18 years and older with documentation of a pain assessment using a standardized tool(s) on each visit AND documentation of a follow-up plan when pain is present |
* The Quality Payment Program was implemented in the U.S. by Medicare in 2017. Merit-based incentive payment system (MIPS) is designed for eligible clinicians who bill under Medicare Part B. Grayed out measures were deleted/retired.
RESOURCES
Official reprint from WoundReference® woundreference.com ©2026 Wound Reference, Inc. All Rights Reserved
Use of WoundReference is subject to the
Subscription and License Agreement.
NOTE: This is a controlled document. This document is not a substitute for proper training, experience, and exercising of professional judgment. While every effort has been made to ensure the accuracy of the contents, neither the authors nor the Wound Reference, Inc. give any guarantee as to the accuracy of the information contained in them nor accept any liability, with respect to loss, damage, injury or expense arising from any such errors or omissions in the contents of the work.
Concise Algorithm for Assessment of Venous Ulcer for use at point-of-care. Comprehensive topic including epidemiology, risk factors, etiology, pathophysiology, history, physical examination, diagnosis, differential diagnoses, documentation and ICD-10 coding. Free Abstract
Summary