Last updated on 12/28/25 | First published on 9/8/21 | Literature review current through Mar. 2026
[cite]
Authors:
Lauren Hayward BA,
Elaine Horibe Song MD, PhD, MBA,
Topic editors:
Erin Tharalson DNP, RN, ANP-BC, CWS,
more...
Coauthor(s)
Elaine Horibe Song, MD, PhD, MBACo-Founder and Editor, Wound Reference, Inc;
Professor (Affiliate), Division of Plastic Surgery, Federal University of Sao Paulo;
Volunteer, Association for the Advancement of Wound Care;
Google Scholar Profile
Disclosures: Nothing to disclose
Lauren Hayward, BA
Disclosures: Nothing to disclose
Editors
Erin Tharalson, DNP, RN, ANP-BC, CWS
Disclosures: Nothing to disclose
WHAT is pyoderma gangrenosum?
Pyoderma gangrenosum is a rare condition that causes large, painful ulcers to appear on the skin. While these ulcers can persist for a long time and come back over and over, they are not contagious.
Pyoderma gangrenosum is most common in adults 20-50 years old. The ulcers are most frequently located on the legs, feet, or trunk, but can occur anywhere on the skin.
The appearance of the condition may vary. The ulcers often start out appearing like pimples, bumps, or blisters, and within a few days can grow in size and open up, resulting in an ulcer which may ooze fluid. The borders of the ulcer may look purple in color and have an irregular shape.
Other symptoms of pyoderma gangrenosum include fever, discomfort, and joint and/or muscle pain.
Below is an example of how pyoderma gangrenosum on the skin can evolve:
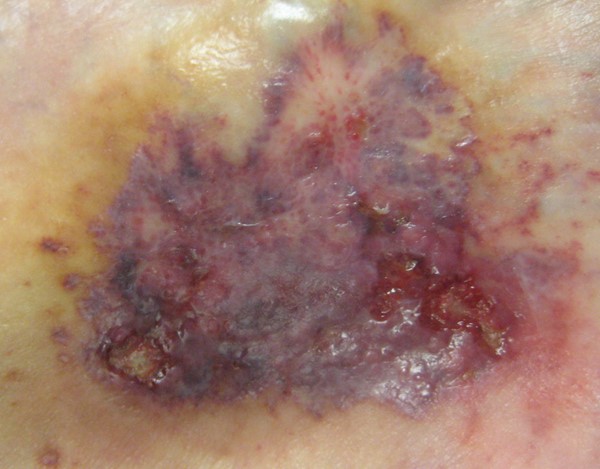
Figure 1. Ulcerative pyoderma gangrenusum, early lesion. By Lebedinskaya N., RN, BSN, CWOCN
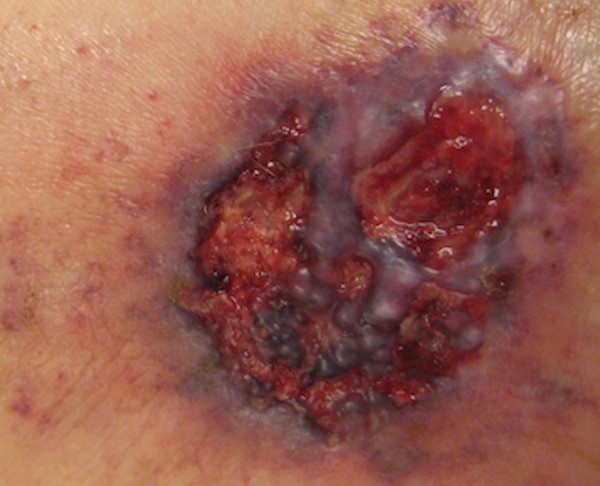
Figure 2. A more advanced ulcerative pyoderma gangrenosum. By Lebedinskaya N., RN, BSN, CWOCN
WHAT causes pyoderma gangrenosum?
The exact cause of pyoderma gangrenosum is not known. In some cases, it may start after a person injuries the skin (cut, burn, bruises, surgery, etc).
Certain conditions are known to be associated with or increase a person’s risk for pyoderma gangrenosum:
- Inflammatory Bowel Disease: People with a digestive tract disease such as ulcerative colitis or Crohn's disease
- Arthritis: People with rheumatoid arthritis
- Blood Disorders: People with acute myelogenous leukemia, myelodysplasia or a myeloproliferative disorder
If you have pyoderma gangrenosum, it does not mean that you have any of these conditions, but your doctor will consider them and take the necessary steps to exclude them.
HOW is pyoderma gangrenosum treated?
Since pyoderma gangrenosum is rare, it can be difficult to diagnose. Often, many tests may be needed to rule out other causes. One of those tests may be a skin biopsy, in which a small sample of skin is taken to be examined under the microscope in a laboratory.
Once diagnosed, treatment for pyoderma gangrenosum depends on how severe the ulcers are.
Figure 3 below shows different methods that may be used to treat pyoderma gangrenosum, based on severity:
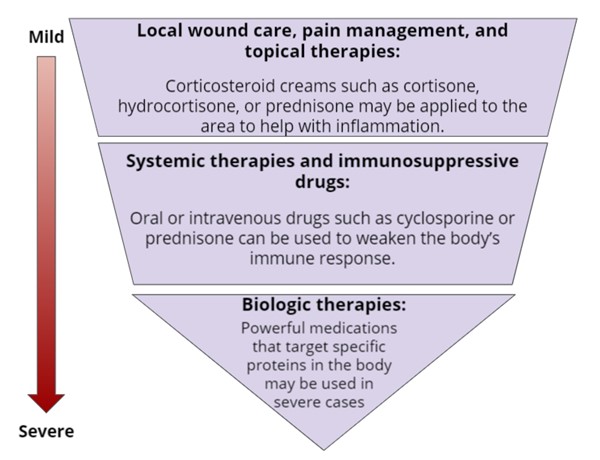
Figure 3. Treatment interventions for pyoderma gangrenosum, based on severity
HOW do I care for my pyoderma gangrenosum?
In order to ensure proper wound healing, consider implementing the following:
- Nutrition Optimization: The body needs plenty of energy from high protein foods to heal properly
- Quit smoking: Nicotine reduces blood flow to the skin, which impairs healing
- Glycemic control: high blood sugar can also reduce blood flow and increase risk of infection
Your clinician will also recommend appropriate dressings to keep the wound area clean and moisturized. Be sure to follow all instructions for changing the dressings in order to avoid infection and promote healing.
WHAT can happen if pyoderma gangrenosum is left untreated?
Pyoderma gangrenosum that is not treated properly can lead to infection, scarring, severe pain, depression, or loss of mobility. With none or limited treatment, healing delays or no improvement may occur.
WHEN should I contact my healthcare provider?
- Don’t wait or hesitate to contact if: you are experiencing new problems or symptoms, your wound begins bleeding excessively, or if you see any signs of infection.
- Signs of infection: fever, nausea, wound redness, warmth, swelling, pain, or a change in wound drainage, odor, or color.
HOW can I prevent pyoderma gangrenosum?
While there is no known way of preventing pyoderma gangrenosum, if you already know you have the condition avoid injury to the skin. Injury or trauma to skin, including surgery, can cause new ulcers to form.
Official reprint from WoundReference® woundreference.com ©2026 Wound Reference, Inc. All Rights Reserved
NOTE: This is a controlled document. This document is not a substitute for proper training, experience, and exercising of professional judgment. While every effort has been made to ensure the accuracy of the contents, neither the authors nor the Wound Reference, Inc. give any guarantee as to the accuracy of the information contained in them nor accept any liability, with respect to loss, damage, injury or expense arising from any such errors or omissions in the contents of the work.